| | |
 |
ARBs. ASN 2002 Satellite Symposium Philadelphia, PA, November, 2002 |
|
00:00

ARBs
Dr. Giles : Its the ACE. I noticed you didnt say anything about that, Matt. And by the way, you cant ask me that question because Im not over 55.
All right. So we are going to talk a little bit about the ARBs. I am going to start out by you know how they always talk about the spin stops here? Well, it is going to stop.
00:00

Development of antihypertensive therapies
If you look at this and you look at the introduction to the ACE inhibitors in the 80s and the ARBs in the 90s, you might ask yourself: What am I talking about spinning? Well, this is where bad science spun a myth. What was the myth? The myth was that ARBs were a natural extension of ACE inhibitors and that they were ACE inhibitors without a cough, with basically nothing whatsoever to support that. In point of fact, the science would support that these two are entirely different classes of drugs. So I think I will demonstrate to you that quite honestly if you want to inhibit the renin angiotensin system and accomplish all of the things that that would do when that system is dysregulated, the ARBs are your choice hands over, for lots of reasons, not the least of which is that they dont cause a problem with side effects.
00:00
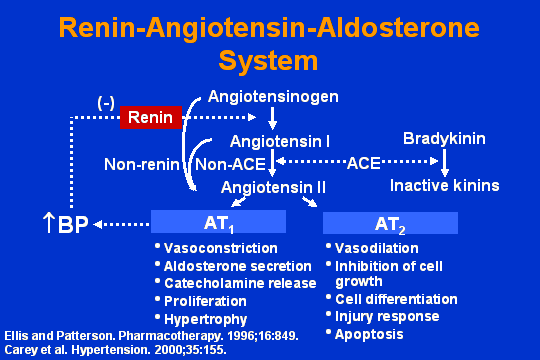
Renin-angiotnesin aldostrone system
Lets look at this cascade for just a second. First of all, if you look at the classic cascade, the converting enzyme is barely a part of the renin angiotensin system. As a matter of fact, the preferred substrate for that enzyme, by the way, is bradykinin. There are 15 substrates for that enzyme; most of them probably have a lot more to do with the beneficial effects of the ACE inhibitors than obviously with reduction of angiotensin-II by this pathway.
There is another little bit of fallacy here and that has to do with the AT-1 receptor and AT-2 receptor subtype. If this room was full of angiotensin receptors and I said, Everybody in here who is an AT-2, raise your hand, I would scarcely find about two of you. So when you start talking about AT-2 receptors being stimulated by angiotensin-II having a lot of effects, that may be some sort of fantasy that people who are purporting to support ACE inhibitors might try to tell you. But if what you want to do is prevent the effects of angiotensin-II at the AT-1 receptor, where it can cause all of this mischief in pathophysiology, what you want to do is actually block the receptor.
00:00
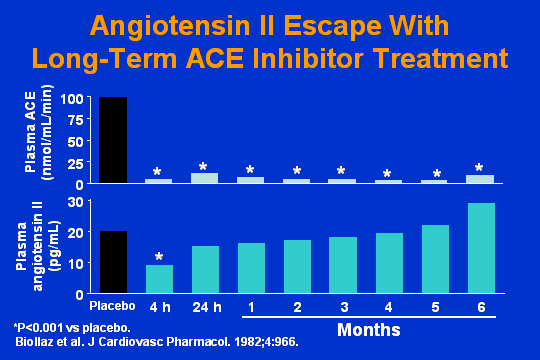
Angiotensin II escape with long-term ACE inhibitor treatment
You are all familiar with slides like this. I only picked this one out to demonstrate what I am talking about. If you take an individual and put him on an ACE inhibitor and you measure plasma ACE activity, what you see is suppression. Six months out, you still have the same degree of suppression. What you dont have is continued suppression of the production of angiotensin-II.
00:00
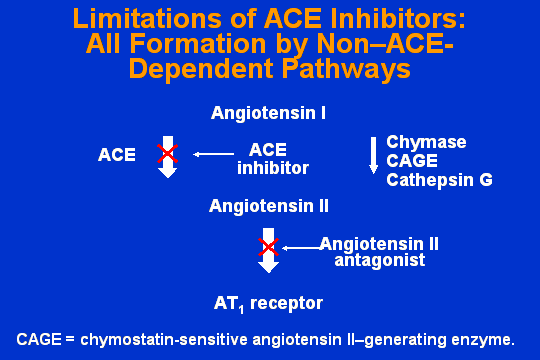
Limitations of ACE inhibitors
The question is: Why does that happen? The reason that that happens is that there are a lot of non-ACE pathways, and particularly in the human, where chymase is responsible in some organ systems for as much as 70 percent of the production of angiotensin-II from angiotensin-I. The problem with my colleague here is I think he has let some rat studies get in the way of his human studies. You see, Matt, the rat doesnt have chymase. And so when you go to look for things like bradykinin stimulation, you have to be very careful. If you are going to look at rats, they have to be two legged. Those are the ones, obviously, that most like the ACE inhibitors. The whole idea is to block the effects of angiotensin-II. The only way you really want to do that is with an angiotensin-II antagonist.
00:00

Genetics of the population
You can look at the genetics of the population, and I think this makes it stand out even more. For example, if you look at how polymorphisms in these whole systems tend to relate to disease, it is interesting. For example, angiotensinogen is one of the gene variants that are most closely related to the development of hypertension. But also there are individuals in the population who have polymorphisms that affect the angiotensin-II type 1-A receptor gene. Furthermore, there are people who have deletion and insertion polymorphisms at the ACE gene, which also dictate how these people will respond to drugs. The reason I am bringing this out is because I am going to show you in a minute and talk to you about the heterogeneity of response when you take a drug, put it into 1,000 people and then guess which one of these genotypes they happen to have.
00:00
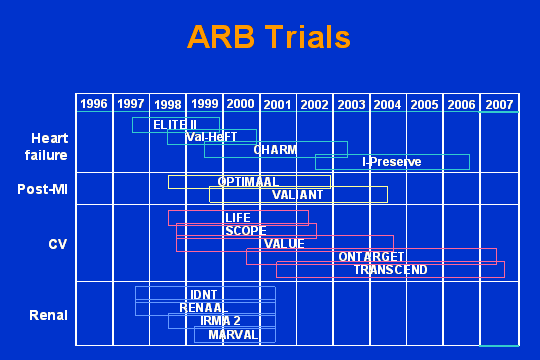
ARB trials
It is not that the ARB people havent been busy. This is a list of the ARB trials, some of them. What I am going to do is go over, in the limited amount of time I have, some of these studies in order to demonstrate a couple of things: First of all, that these drugs are safe and effective; but secondly to show you in some context how the development of this class of drugs has been impeded by the time at which they were introduced.
00:00

Heart failure
First of all, lets look at heart failure. This is where I think there has been a little misadventure, I think, that took us down a pathway that some people have taken advantage of, and I would like to set the record straight a little bit. I am going to show you data from ELITE-2 and from the Val-HeFT study, which both looked at patients who had reduced ejection fractions and were Class II to IV heart failure. This is the New York Heart Association classification. They were fairly substantially large studies. One had a little over 3,000 patients, and one having over 5,000. The differences in these two trials were as follows. ELITE-2 was a trial designed to compare the angiotensin receptor blocker, losartan, versus captopril, doses as you see here, on all-cause mortality. Val-HeFT was a trial that was conceived with ELITE-2 in mind because in this trial ACE inhibitors were permitted, whereas in ELITE-2, most of the patients were ACE naïve. Therefore, in the angiotensin receptor blocker valsartan was added to digoxin, diuretics, and 93 percent of the people were taking an ACE inhibitor. All-cause mortality and combined morbidity and mortality comprised two primary endpoints.
00:00
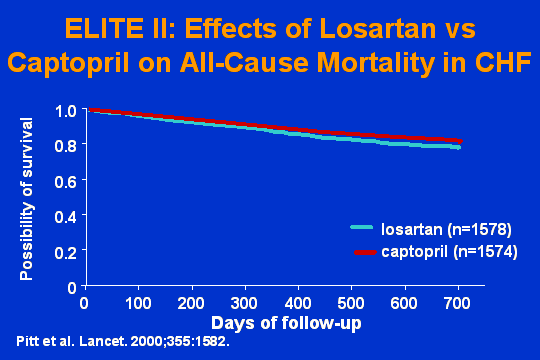
ELITE II trial
This trial was designed as a superiority trial. Those of you in here who are statisticians will know that in order to draw conclusions from this trial, one would have had to have the ACE inhibitor and losartan compared in such a way that there would be non-inferiority or comparability. The trial was not designed that way. So you say, What do we do with these data? I would suggest to you that this survives the British BOD study. What is the obvious difference? There is no difference between these two. I mean, anybody who says there is a difference between those two is using statistics like a drunk uses a lamp postmore for support than for illumination. What you have here is comparability.
00:00
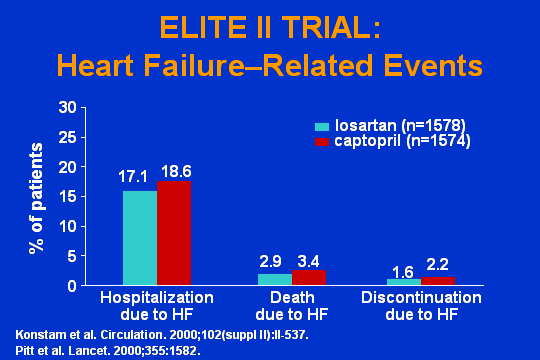
ELITE II trial: Heart failure
As a matter of fact, if you look at every one of these outcomes, whether it is hospitalization, death due to heart failure, discontinuation due to heart failurethey are comparable. The ARB is just as good as the ACE.
00:00
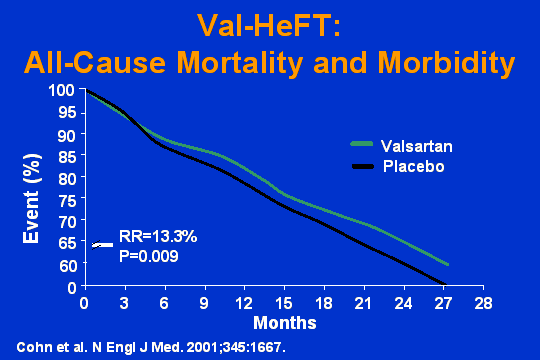
Val-HeFT
Lets look at Val-HeFT . All-cause mortality and morbidity. This is what happens when you add an ARB to somebody who is already taking an ACE. And you get this nice 13 percent reduction, highly statistically significant in all-cause mortality and morbidity.
00:00
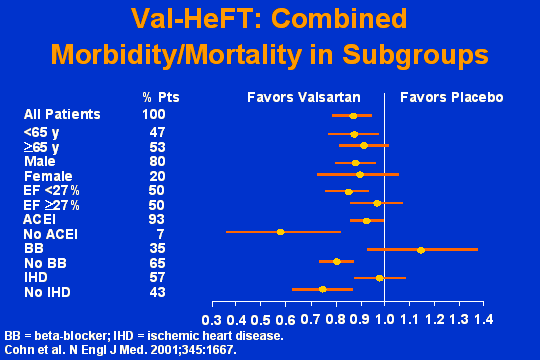
Val-HeFT
Now lets look at the subgroups. And what jumps out at you is this group. And who is this? These are the people who were not taking an ACE inhibitor. This is your totally ACE-naïve patient who has now gotten an angiotensin receptor blocker and moves not only the point estimate but these 95 percent confidence intervals so far over that I think that together with ELITE-2 tells you clearly that the angiotensin receptor blockers are effective.
00:00

ARB megatrials in cvd
There are some other trials, and I will show you some data from those, too, in cardiovascular disease. The LIFE trial, I think, is probably one of the more important trials that we have had in the last 5 or 10 years, particularly relative to this class of drugs. The populationpeople with high blood pressure and left ventricular hypertrophy, 9,000 of them as a matter of fact, and the treatment regimen compared a losartan-based therapy versus an atenolol-based therapy with the primary endpoint being an acute MI, stroke, or cardiovascular death.
00:00
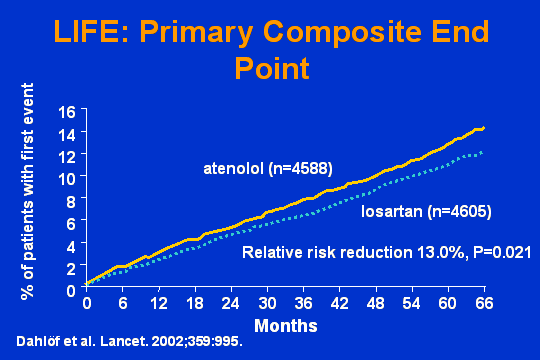
LIFE trial
These are what the data look like. Here is the primary composite endpoint. Again, losartan had a risk reduction of 13 percenthighly statistically significantcompared to atenolol-based therapy in this group of patients. They are over 55, by the way, Matt.
00:00
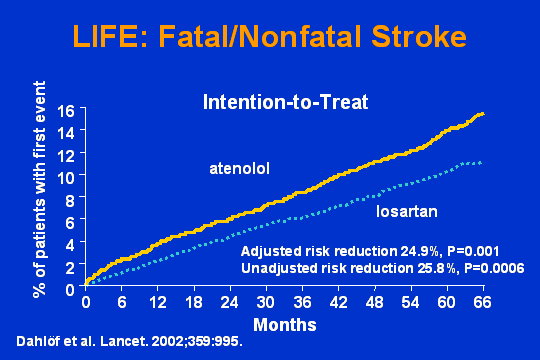
LIFE: Fatal/nonfatal stroke
What about stroke? Highly statistically significant. Here is the atenolol group. Here is the losartan group. Once again, about a 25 percent reduction in stroke losartan versus atenolol.
00:00
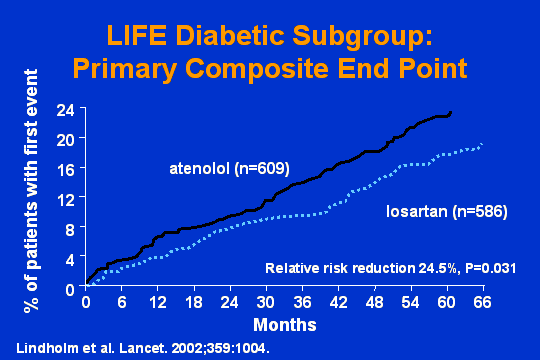
LIFE: Diabetic subgroup
How about in the diabetics? Here is the primary composite endpointan even greater reduction. Here is a 25 percent relative risk reduction in the primary composite endpoint, losartan-based therapy versus atenolol. And by the way, atenolol, beta blockersone of the best anti-renin drugs we have ever had.
00:00
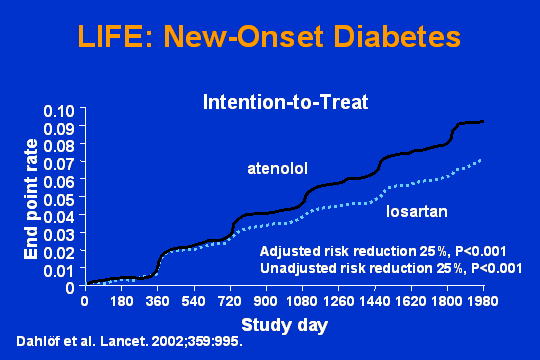
LIFE: New-onset diabetes
New onset diabetes. I will grant that there are some studies, HOPE being one of them, the Captopril Prevention Study being another, that have shown data similar to this. But here is losartan demonstrating on an intention-to-treat analysis a 25 percent reduction in new onset diabetes. You block the effects of angiotensin-2, and there are adverse effects on the beta cells of the pancreas, number one. And two, you reduce all the problems with microvascular flow to skeletal muscle, and that is the payoff.
00:00
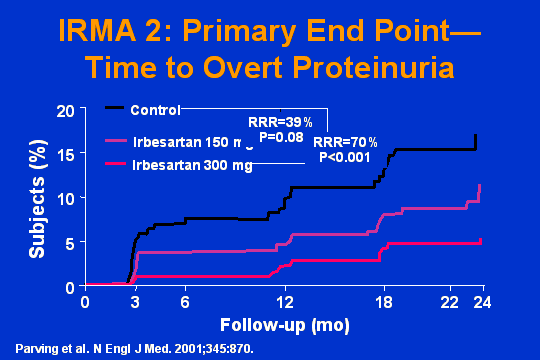
IRMA-2 primary endpoint
I was warned by Dr. Bakris that I could spend one minute on the next three slides. So I am going to do that. Here is IRMA-2, primary endpoint, time to overt proteinuria. Who wins? The ARB.
00:00
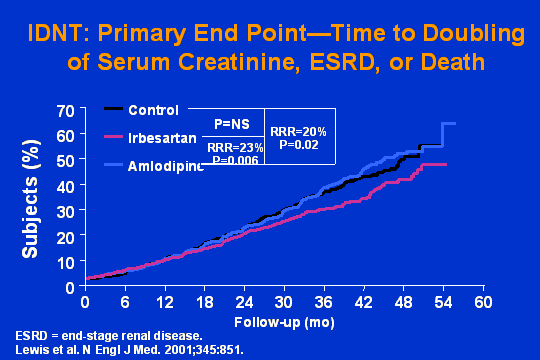
LIFE: Time to doubling serum creatinine
Here is IDNT , primary endpointtime to doubling of serum creatinine, end-stage renal disease, or death. Who wins? Certainly not control. Certainly not amlodipine. The ARB.
00:00
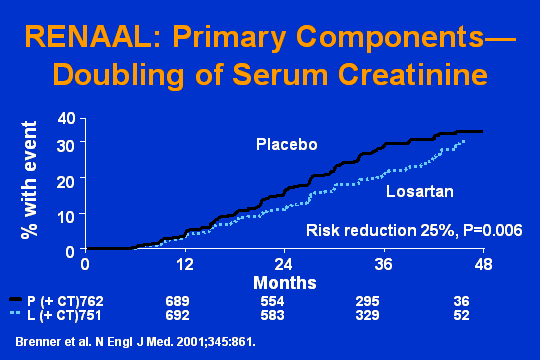
RENAAL
Here is RENAAL. Primary componentsdoubling of serum creatinine. Placebo, losartan. Dr. Brenner has already shown you. Who wins? The ARB.
Now here is the thing that Dr. Weir totally forgot about. You see, when a patient walks into your office, you have two issues, right? One thing is you want to make them feel better, you want to make them live longer, but you dont want to hurt them. Right? You dont want to make them sick. You dont want to have them come back in the middle of the night to be intubated. You dont want their tongue to swell up, right, and become rigid right in front of your eyes. You dont want them to come in and have their wife run you out because now her husband coughs incessantly and never stops. So what about the safety of the ARBs? Probably the only class of drugs that have ever been around in cardiovascular medicine since I have been there that have a side effect profile that is virtually indistinguishable from placebo.
00:00
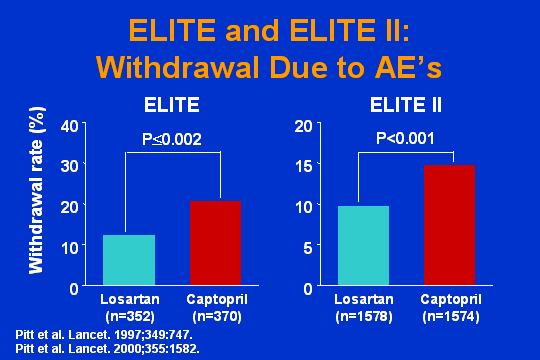
ELITE and ELITE II
In the clinical trials that I just showed you, here is the withdrawal due to ACE. Once again, here is captopril. That is an ACE inhibitor. Right in here. The one that is kind of high here. That is the blue one down there.
00:00
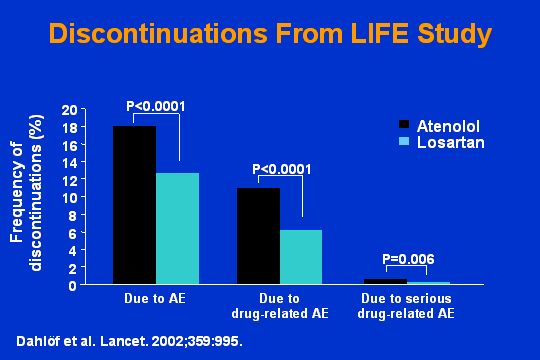
Discontinuations from LIFE study
And in the LIFE study, the same thing. Here is atenolol. Here is losartan. And you can see in every one of these categories the beautiful side effect profile.
00:00

Advantages of ARBs
So here is how I would phrase it. Here are the advantages of the angiotensin receptor blockers. First of all, if you want to block angiotensin-2, the science would support that the way you do that is you block the receptor. Secondly, there is placebo-level tolerability. You might get a little bit of bradykinin, but I will tell you it aint much. There is no ACE inhibitor related cough. Secondly, stimulation of the AT-2 receptor may be associated with some benefits. I havent had time to show you that. I think the future guidelines making for lower blood pressures are going to emphasize that you need drugs you can give people that they will actually take.
00:00

Advantages of ARBs(continued)
There is clinical trial evidence demonstrating efficacy in lowering blood pressure. I didnt have to show you that. I think I showed you clearly that they are effective in the treatment of heart failure. The reduce stroke in patients with hypertension and LVH and clearly have renal and cardio protection in hypertensive diabetics.
Thank you.
References
1. Carey RM, Wang ZQ, Siragy HM. Role of the angiotensin type 2 receptor in the regulation of blood pressure and renal function. Hypertension 2000 Jan;35(1 Pt 2):155-63.
2. Biollaz J, Brunner HR, Gavras I, Waeber B, Gavras H. Antihypertensive therapy with MK 421: angiotensin II--renin relationships to evaluate efficacy of converting enzyme blockade. J Cardiovasc Pharmacol 1982 Nov-Dec;4(6):966-72.
3. Cohn JN, Tognoni G, et al. A randomized trial of the angiotensin-receptor blocker valsartan in chronic heart failure. N Engl J Med 2001 Dec 6;345(23):1667-75.
4. Pitt B, Poole-Wilson PA, Segal R, Martinez FA, Dickstein K, et al. Effect of losartan compared with captopril on mortality in patients with symptomatic heart failure: randomised trial--the Losartan Heart Failure Survival Study ELITE II. Lancet 2000 May 6;355(9215):1582-7.
5. Dahlof B, Devereux R, de Faire U, Fyhrquist F, Hedner T, et al. The Losartan Intervention For Endpoint reduction (LIFE) in Hypertension study: rationale, design, and methods. The LIFE Study Group. Am J Hypertens 1997 Jul;10(7 Pt 1):705-13.
6. Mann J, Julius S. The Valsartan Antihypertensive Long-term Use Evaluation (VALUE) trial of cardiovascular events in hypertension. Rationale and design. Blood Press 1998 May;7(3):176-83.
7. Dahlof B, Devereux RB, Kjeldsen SE, Julius S, Beevers G, et al. Cardiovascular morbidity and mortality in the Losartan Intervention For Endpoint reduction in hypertension study (LIFE): a randomised trial against atenolol. Lancet 2002 Mar 23;359(9311):995-1003.
8. Lindholm LH, Ibsen H, Dahlof B, Devereux RB, Beevers G, et al. Cardiovascular morbidity and mortality in patients with diabetes in the Losartan Intervention For Endpoint reduction in hypertension study (LIFE): a randomised trial against atenolol. Lancet 2002 Mar 23;359(9311):1004-10.
9. Parving HH, Lehnert H, Brochner-Mortensen J, Gomis R, Andersen S, et al. The effect of irbesartan on the development of diabetic nephropathy in patients with type 2 diabetes. N Engl J Med 2001 Sep 20;345(12):870-8.
10. Lewis EJ, Hunsicker LG, Clarke WR, Berl T, Pohl MA, et al. Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N Engl J Med 2001 Sep 20;345(12):851-60.
11. Brenner BM, Cooper ME, de Zeeuw D, Keane WF, Mitch WE, et al. Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med 2001 Sep 20;345(12):861-9.
12. Pitt B, Segal R, Martinez FA, Meurers G, Cowley AJ, et al. Randomised trial of losartan versus captopril in patients over 65 with heart failure (Evaluation of Losartan in the Elderly Study, ELITE) Lancet 1997 Mar 15;349(9054):747-52.
13. Ellis ML, Patterson JH.A new class of antihypertensive therapy: angiotensin II receptor antagonists. Pharmacotherapy 1996 Sep-Oct;16(5):849-60.
14. Pylypchuk GB. ACE inhibitor- versus angiotensin II blocker-induced cough and angioedema. Ann Pharmacother 1998 Oct;32(10):1060-6.
15. Carey RM, Wang ZQ, Siragy HM. Role of the angiotensin type 2 receptor in the regulation of blood pressure and renal function. Hypertension 2000 Jan;35(1 Pt 2):155-63.
|
This educational activity is supported by an educational grant from Merck and Company. This activity has been planned and produced in accordance with the HSCCME Essential Areas and Policies. This educational activity is based on a Satellite symposium held in November, 2002 at The 35th Annual Meeting of the American Society of Nephrology in Philadelphia, PA. This symposium was approved by ASN. It was not part of the official ASN Annual Meeting. |
| |||||||||||||||