|
|
|
 |
The Advancement of Clinical Practice in Chronic Kidney Disease RPA Satellite Symposium March 22, 2002 Correcting Anemia: Improving Renal and Cardiovascular Outcomes |
|
Dr. Anton Schoolwerth:
Let's move on then to our next speaker. Dr. Reddan is going to speak to us about correcting anemia, improving renal and cardiovascular outcomes. Dr. Reddan?
00:00

Dr. Donal Reddan:
Thank you very much. I'd like to thank Ortho Biotech for the opportunity. I'd also like to let you know that I haven't heard any news from Ajay yet but we're all hoping for the best. So my task today is to talk about what we know about treating anemia in chronic kidney disease and its effect on clinical outcomes. So far I think the most important point to make at the outset is that the data that are currently available as to better clinical outcomes following anemia correction in patients with chronic kidney disease are quite sparse.
00:00

Benefits of treating anemia of CKD
Here are a list of the number of areas in which there is at least some data. We know from multiple retrospective analyses that there is quite a significant association between mortality and anemia in chronic kidney disease and in ESRD. The most recent data from Allan Collins showing an association between different levels of anemia and mortality are important. When he looked at USRDS data and grouped patients by cohort of anemia into hematocrits less than 30, 30 to 33, 33 to 36 and 36 and above, when he compared patients with those with hematocrits less than 36, he was able to show a significant association with a reduction in hospitalization and also reduction in costs.
There was a 16 percent reduction in hospitalization rate in patients with hematocrits over 36 when compared with patients with hematocrits less than 36 and an 8 percent reduction in costs. There was no significant difference in mortality between the two groups. And it's important to point out that pretty much all the data with respect to all of these clinical outcomes is retrospective data.
With regard to reduction in cardiovascular disease there's very little data as to the effect of anemia correction on ischemic heart disease. And there are two small studies with regard to left ventricular hypertrophy that Dr. Al-Ahmad already mentioned and I'll go into a little bit in detail later. With regard to improvement in well being I think this is really where we have the best data. There is pretty conclusive evidence in a CKD population and also in other spheres of medicine such as oncology that anemia correction really does improve quality of life.
I think the best data in this area in chronic kidney disease is from Revicki's study which looked at 85 patients with chronic kidney disease in a randomized controlled trial and they were able to demonstrate significant improvement in physical activity and also in cognitive function in patients with chronic kidney disease. There were two or three other good studies that showed improvement in cognitive function with anemia correction of chronic kidney disease and this is also consistent with data showing EPO receptors in the brain which may suggest that EPO may have other effects other than the anemia benefit.
There's ESRD data showing improvements in sleep patterns and also some anecdotal data in the CKD population. And in addition to the data from Dr. Collins that showed an association with reduced hospitalizations in this population from anemia correction, also other data from Neil Powe which shows pretty much the same thing. Again, retrospective data. And this renalpause. Ajay put that in there so I have to explain it. There's also anecdotal to suggest that female patients with chronic kidney disease have menstrual abnormalities. Sometimes those menstrual abnormalities can improve with correction of anemia.
00:00
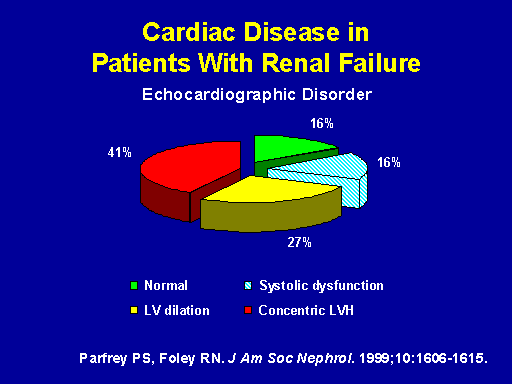
Cardiac disease in patients with renal failure
So how about the prevalence of cardiac disease in patients with renal failure? This data is from Pat Parfrey and looks at incidence in an ESRD cohort of 432 patients. The most important statistic here is that only 16 percent of these patients had normal echocardiograms at the time of initiation of hemodialysis. Forty-one percent of the patients had concentric LVH, 27 percent had LV dilatation, and 16 percent had evidence of systolic dysfunction. Levin has similar data looking at a chronic kidney disease population, GFRs less than 25. She demonstrated a prevalence of concentric left ventricular hypertrophy of 25 percent in that population.
As for coronary artery disease there are numerous small series looking at the prevalence of coronary artery disease in patients before they start dialysis. Again they show an increase in prevalence relative to normal patients. As Dr. Parfrey pointed out, this could just very well be a surrogate for the fact that these patients are generally sick and have a lot of comorbidities. And it's difficult to ascertain whether the renal failure itself is the cause of the increase in coronary artery disease.
00:00

Predictors of left ventricular hypertrophy
This is a small study by Greaves looking at the predictors of left ventricular hypertrophy. This is a study from the mid-90s that looked at echocardiographic data on 181 patients at various levels of renal insufficiency. Thirty-eight patients had chronic renal insufficiency. Approximately 50 patients were on dialysis and 40 patients on peritoneal dialysis. There were also a number of control patients in the group as well.
And when patients with chronic renal insufficiency were compared with patients who were normal controls there was a significant increase in their left ventricular mass index. There was also an increase in left ventricular mass index in the patients who were receiving renal replacement therapy relative to the controls. And within the CKD population the various factors that were found to be associated with LVH included anemia, hypertension and diabetes.
00:00
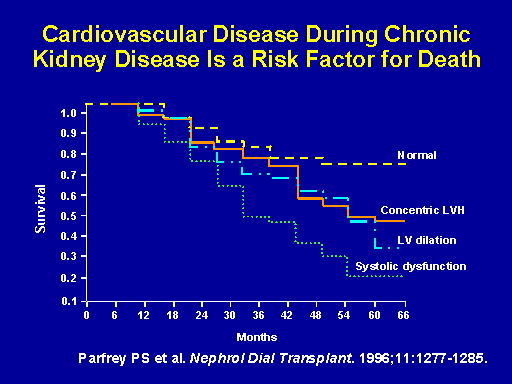
Cardiovascular disease during chronic kidney disease is a risk factor for death
When we look at the mortality risk associated with having various left ventricular geometric abnormalities, this is the same cohort that Pat Parfrey described per the earlier slide I presented with the pie chart showing the various prevalence of the left ventricular geometric abnormalities in the ESRD cohort. Of these 432 patients, when you divided the patients into the various different levels of cardiac abnormalities: normal cardiac geometry, concentric LVH, LV dilatation and systolic dysfunction ... you can see that the patients with echocardiographic abnormalities have significantly increased mortality compared with patients that have normal echos.
00:00
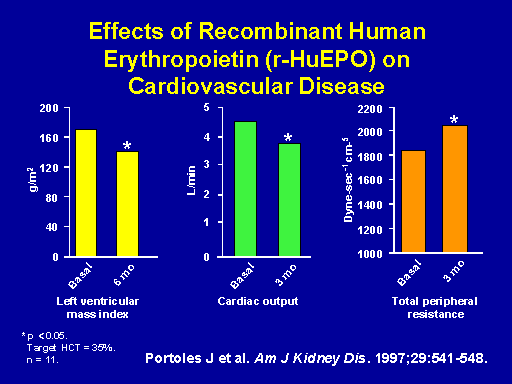
Effects of recombinant human erythropoietin (r-HuEPO) on cardiovascular disease
This is one of the two studies that Dr. Al-Ahmad mentioned earlier. This is Portoles paper. Again, just to reinforce that this study has 11 patients; the next one will have 16 patients. No control groups. And neither study was a randomized controlled trial obviously and so they weren't powered. So I think really we have to take all of this data as purely hypothesis generating. Just to summarize quickly, the Portoles data showed that in patients who were treated for six months with anemia correction LV mass index showed a significant reduction. Also cardiac output showed a significant reduction and total peripheral resistance showed a significant increase.
00:00
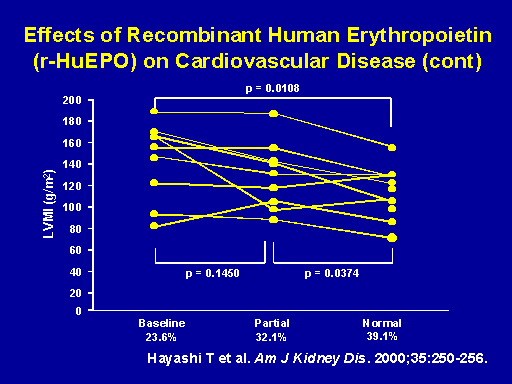
Effects of recombinant human erythropoietin (r-HuEPO) on cardiovascular disease (cont.)
This is the Hayashi paper. These patients were treated for 12 months. At 4 months there was a trend but not a significant difference in LV mass index. At 12 months there was a significant decrease in LV mass index with anemia correction. Again, 16 patients in this study so it really is just hypothesis generating. As Dr. Parfrey pointed out there are a number of studies ongoing that should help to answer this question. We also hope to answer this question with the CHOIR study as we're planning to do a sub-study of 300 patients that will hopefully answer this question once and for all as to whether anemia correction improves LV mass index.
00:00

CHOIR hypothesis
So now I'm to the CHOIR study. Before going into the CHOIR study I just wanted to acknowledge the energy and enthusiasm of our current RPA President, Bill Owen, in getting this going. Also the hard work by Ajay and Ly-le Tran from Ortho Biotech with regard to getting the study going. I think we're all excited. It's about to start enrolling patients in the next few days actually. So this is quite an exciting time for us. The hypothesis underlying the CHOIR study is that the level of anemia correction with once weekly dosing of recombinant EPO in patients with chronic kidney disease will decrease mortality and cardiovascular morbidity.
00:00

Study design
This is to be a randomized, controlled study. It's an open-label study, 150 sites, 4-years duration, 2,000 patients.
00:00

Study population
The study population includes patients with hemoglobins less than 11, age greater than 18 years and a steady state GFR between 15 and 50 ml per minute. Now, I think as Dr. McClellan's data pointed out earlier, we expect that the majority of the patients with hemoglobins less than 11 will have GFRs probably 30 and below. But we are including patients up to a GFR of 50.
00:00

Study treatments
The study will involve treatments in two separate arms. One arm will involve therapy directed to achieving hemoglobin of 13.0 to 13.5 g/dl. And this will involve EPO therapy once weekly to this target with doses adjusted accordingly. The lower arm will involve therapy directed to maintain a hemoglobin of 10.5 to 11.0 g/dl. Again, this will involve once weekly therapy adjusted accordingly to that target.
00:00

Study timeline
The study timetable will involve one year for patient accrual and 36 months for patient intervention. Patients who initiate renal replacement therapy will be discontinued from the study at the time of initiation of renal replacement therapy. The closeout phase of the study will take about three months after intervention has been completed in all of the patients.
00:00

Primary outcome
Primary outcome of this study includes mortality, myocardial infarction, stroke and CHF hospitalization. And obviously when you design a study like this the most important outcome is mortality. The reason we have a composite outcome is primarily for power reasons.
These latter three components of the primary outcome will be adjudicated by an independent clinical events committee. What that means is that every time an event is suspected at a site, a folder will be sent for evaluation at the clinical research organization level and then the event will be evaluated by an independent committee of physicians who will then determine based on very strict criteria, whether an event has taken place or not. This adds an awful lot of objectivity to these endpoints and really hardens them up because this is a really important study and we need hard clinical outcomes in order to make it worthwhile.
00:00

Secondary outcomes
Secondly outcomes will include each of the components of the primary outcomes individually and will also include hospitalizations, renal function, nutrition and quality of life. With respect to renal function as you know there is some data that suggests that perhaps anemia correction in this population may delay the progression of renal disease. I think this is one of the components of the study that we truly have equipoise on as there is evidence on both sides of that fence. There is evidence that suggests possibly that anemia correction may slow the progression and there's also a little weaker evidence that it may actually hasten the progression. So I think this is another opportunity that the study gives us to answer hard clinical outcomes.
00:00

Exclusion criteria
We exclude patients with uncontrolled hypertension. We also exclude patients with iron overload. We also exclude patients with unstable angina pectoris or angina at rest. This is primarily to avoid some of the problems that we think may have taken place in the other large normalization of hematocrit study in ESRD patients. We think by excluding patients with unstable angina pectoris or angina at rest we may exclude some of the very high risk patients and therefore not compromise our outcomes. We exclude patients with refractory iron deficiency anemia. And we also recommend within the protocol that patients be maintained in an iron replete state using appropriate iron repletion with either oral or IV iron therapy. Patients are also excluded from the study if they are currently receiving recombinant erythropoietin or if they have received it within three months of study entry.
00:00

Anemia and chronic kidney disease conclusions
So in conclusion I think we can say that the CKD population like the ESRD population is probably susceptible to a significant increase in cardiovascular risk. Modifying the chronic kidney disease risk factor of anemia as well as other risk factors as some of the other speakers have pointed out may possibly improve outcomes. And we think the CHOIR study will help to answer a lot of the unanswered questions in this population by focusing on clinical outcomes in an important way to answer these questions. Thank you very much.
References
1. Parfrey PS, Foley RN. The clinical epidemiology of cardiac disease in chronic renal failure. J Am Soc Nephrol. 1999 Jul;10(7):1606-15. Review. No abstract available.
2. Greaves SC, Gamble GD, Collins JF, Whalley GA, Sharpe DN. Determinants of left ventricular hypertrophy and systolic dysfunction in chronic renal failure. Am J Kidney Dis. 1994 Nov;24(5):768-76.
3. Parfrey PS, Foley RN, Harnett JD, Kent GM, Murray DC, Barre PE. Outcome and risk factors for left ventricular disorders in chronic uraemia. Nephrol Dial Transplant. 1996 Jul;11(7):1277-85.
4. Hayashi T, Suzuki A, Shoji T, Togawa M, Okada N, Tsubakihara Y, Imai E, Hori M. Cardiovascular effect of normalizing the hematocrit level during erythropoietin therapy in predialysis patients with chronic renal failure. Am J Kidney Dis. 2000 Feb;35(2):250-6.
5. Portoles J, Torralbo A, Martin P, Rodrigo J, Herrero JA, Barrientos A. Cardiovascular effects of recombinant human erythropoietin in predialysis patients. Am J Kidney Dis. 1997 Apr;29(4):541-8.
| This educational activity is supported by an educational grant from Ortho Biotech Products, L.P. This activity has been planned and produced in accordance with the ACCME Essential Areas and Policies and with CE policies of the State of California Board of Registered Nursing. From a CME Symposium held on March 22, 2002 at the Renal Physicians Association (RPA) Annual Meeting in Washington, DC. This symposium was approved by the RPA. It was not part of the official RPA Annual Meeting as planned by the RPA Program Committee. |
| |||||||||||||||