|
|
|
 |
 |
 |
| |||||||||||||||||||||||||||||||||||||||||||
00:01

Introduction
Our next speaker is Betsy Copeland and Betsy is a Certified Advanced Practice Registered Nurse. She has been practicing at a variety of parts of nephrology for over 7 years, and she is a speaker for American Regent and also for Amgen and her emphasis is on anemia management.
Ms. Copeland
As Dr. Reed has clearly shown you, anemia and iron deficiency are significant in the CKD population, IV iron is more efficacious than oral iron, and our outcomes for the patients, which is what is most important, are better when they are seen in the CKD Clinic and their anemia is managed properly. And while we would love to stand here and look at those outcome slides and go like, "Oh yeah, it was easy," or "Good, go have fun," we cannot do that because it was hard, and as with everything in nephrology, and medicine in general, you are always going to face obstacles. It is always going to be difficult. So what I hope to do is talk to you about some of those obstacles and break them down, and tell you some things that we learned; but then also, tell you some obstacles that are continuing to be faced, that you will face, and that will continue and always will be a challenge.
Before I get started on that, I will ask a few questions just so we kind of have an idea of exactly whom I am talking to. By show of hands, how many of you are primarily hemodialysis nurses? You all work hard! How many are primarily peritoneal dialysis nurses? You all work hard too! I did not realize that until I started working with some of the peritoneal dialysis patients as a nurse practitioner. How many of you do not work in hemodialysis or peritoneal dialysis but you work in the predialysis clinic with the nephrologist? Good, there are a few! For the majority of you who are in hemodialysis and peritoneal dialysis and do not work with the predialysis population, you might be saying, "Well, what does this really have to do with me? I'm not going to be doing this." We are going to talk about that some, and he has already addressed that a little bit of how it affects your patients when you see them. What it means when they walk in the door to you. Another thing about that is - our office - I worked on the hemodialysis floor before I went back to school to become a nurse practitioner. The RN in our office was a tech on the hemodialysis floor. Then she went to nursing school. She was a nurse in hemodialysis, and now she is an RN in our office. We had to get her some help when we started getting all this other work. She has a tech who worked a very, very long time on the hemodialysis floor. So, I do not want any dialysis managers throwing anything at me because it sounds like I am trying to steal your workers, but we all know that there is crossover. We all make changes in our career from time to time, so nothing better in the predialysis clinic than an experienced dialysis nurse or tech to help us work with the patient, so that is another side of why it could be important to you.
03:02

Obstacles to treatment success
Some of the obstacles. We will talk about timely referral - Dr. Reed touched on that a little bit - of non-dialysis dependent CKD patients. We are going to talk about finding the time in your daily practice. I am sure if I asked each of you, okay I need you to do one more hour's worth of work in the time you are already doing, you would all laugh in my face. There is never enough time to do what we are doing, so how do we change our focus and make the time for that? I will talk about some real world obstacles, just a few little nuts and bolts of day in, day out treatment with iron therapy and then the availability of the erythropoietin, and now the availability of the IV iron agents, in the CKD clinic.
To back up, start with the timely referral. Well, our focus and the focus of nephrology is really shifting to the CKD clinic. Through the years, the main focus has been on the hemodialysis and peritoneal dialysis. The shift is to look at the CKD clinic, the predialysis population, and get them ready. We realized that we had come to that conclusion that we were ready to make that shift but then all of a sudden, we realized - Wait a minute! The family practice physicians, primary care physicians, their nurse practitioners and internists, they have not made that shift yet. We still were not getting the patients in time to make a difference. If you think, you have to have the patients to actually treat the anemia and iron deficiency and make a difference. So, we decided we needed to something about that. We looked to see why are we not getting the patients? What is the problem? What is the big deal?
04:31

Causes of late referral
This was a study published in Dialysis and Transplantation: They did a survey; they asked the primary care physicians why they were not sending patients to nephrology. In 50% of cases it was simply a lack of communication with the nephrologist, a result of poor talking. About 40% feared being negatively evaluated by a nephrologist. There is not one of us who wants to do our best and do what we can for the patient and then the patient goes to somebody else. The other person will say, "Why were you not doing this, this, and this?" They did not want to look bad, and we can all understand that. About 90%, though, were just unfamiliar with the guidelines. About 90% just said, " I don't know any one of them. I don't know what I am supposed to look at specifically to send patients to you."
05:19
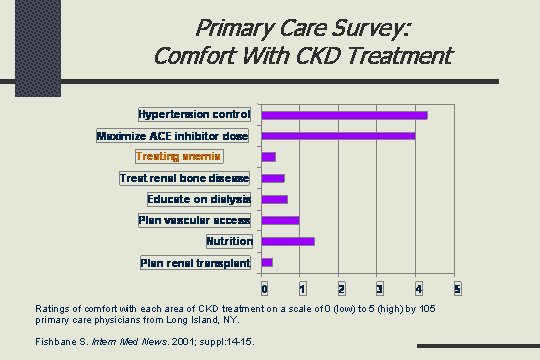
Comfort with CKD treatment - survey
In addition to that, another survey was done to ask the primary care physicians - what are you most comfortable with? When you are treating a predialysis patient, what do you feel comfortable with, and they were to rate it on a scale of 0 to 5, 0 being their lowest comfort level and 5 being their highest. As you see, hypertension control, they were very comfortable with. They knew that. That was what they do day in, day out. They were very comfortable with maximizing the ACE inhibitor dose. As you come down to some of the others, treating anemia is very low. This is just barely above renal transplant, and so they did not know anything about anemia treatment. What we did is we decided to get out there and tell them, since that is something that we knew about.
06:04
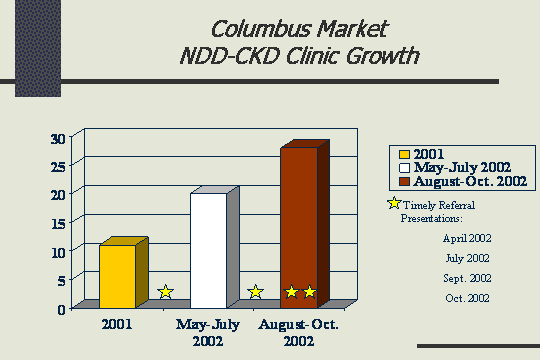
Columbus market NDD-CKD clinic growth
What this illustration shows is that over a very short period of time, we decided to go communicate with these internists. It was a novel idea but we were going to go and talk to them and just let them know what we are here for, and we did lunch presentations and dinner presentations. We gave them a good steak and asked them to listen to us for a little while, and we just told them. Dr. Reed stood up in front of them very humbly - these physicians with whom he has worked for years and said - "okay guys, it is different now". Before I told you to send me the patient when the patient was vomiting or could not breathe. Things are different now. I have help, and we have new treatment, and we can do a better job, so let us do it. We told them the guidelines as far as calculating the GFR from the creatinine. We told them what we could do in terms of anemia management; and how, by building the relationship and the trust with the patient, we were able to get an access placed. Patients were able to start dialysis without walking into the hospital. And if you could see by the stars, the stars indicate a presentation, our monthly average referrals tripled after only 4 presentations. Just tell somebody what they need to do, and most people are going to do it. They just need to know.
07:19
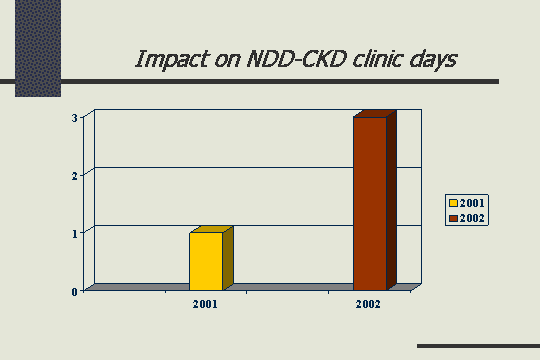
Impact on CKD-NDD clinic days
That is when it got interesting, because that is when we had the significant impact on that focus change that we were wanting to make. In 2001, there was like one day a week that we had the clinic for the predialysis patients. We had to increase that to 3 days a week, and that is a pretty big change when you think about day in, day out, how you are going to make the schedule work. It did.
07:42

Where did we find the time?
Where did we find the time? Initially, we did not. Initially, the physicians were overloaded. We were pulling them in 500 different directions, schedule was tight, it was frustrating, and so early on, a nurse practitioner was added to help and stabilize the CKD clinic just for the followups, and also to help some with the time constraints of the hemo rounding and that kind of thing, for a length of time. What we found, as Dr. Reed talked about, was that once we started getting the referrals, once we started seeing the patients early, we had less hospitalizations. There were fewer of those midnight calls with a creatinine of 11 and hemoglobin of 7. That freed up some time, not to mention sleep, and we were better able to provide the care that we needed to provide. So, one thing I really want to get across to you guys is we found the time in that our acuity level in the limited care units changed.
Work in the hemodialysis floor - you know what it is like to have that patient come in from the hospital with 3 or 4 pages of hospital orders, hemoglobin is low, who feels horrible, vomiting, everything is awful. You know how many times, I do not work where you work, but the physician has to be called and asked about something or the physician has to be brought in to see the patient, so you are going to need to go back to the hospital. We found that by treating these patients in the predialysis setting, they did not go to the hospital. It was a joy to see a patient that you have been seeing even like he said for 3-4 months and see that patient walk into the dialysis unit the first day, have an access in the arm, and I am not saying everybody did because they did not, but you know possibly an access so you can at least get one needle in, and their anemia being in target and they are feeling okay, so they are laughing and joking around and they are feeling better. I am not saying everybody because we all know it is a big life adjustment, but there was definitely a difference in that patient who came from the CKD clinic first of all compared to one who came from the hospital. What does that mean to you? A lot easier patient to take care of day in, day out, so that is just one thing I wanted to get across to you, why we really want to talk to you guys about this. So that when you go home, if your nephrologists are not already doing this, you can say - if you do this, this will make both of our lives easier, not to mention the most important thing, it is better for the patient. Now, one other question to ask. (I'm trying to keep them wide awake!) How many of you work with a nephrologist who has an active predialysis CKD clinic and who treats anemia in that clinic? I am bad at numbers, maybe half, just maybe a little bit more. That is something we need to understand a little bit better; what your nephrologists are trying to do, and if they are not, to go back and ask them - Why not?
10:23

"Real world" obstacles
The real world obstacles. When we began using the IV iron, we began the infusions in the outpatient hospital setting. To be honest with you, we ran across a lot of challenges with that. Patient compliance and convenience was an issue. The patients would go to the outpatient center and while receiving the actual iron did not take long - they would be forced to sit in the waiting room 3-4 hours and they were frustrated. They have already to come to see us one day here and there, we got them going for a vein mapping, we got them going here, then we send them to the hospital to sit for 3-4 hours to get iron, so that was an issue. Educating the pharmacist at the hospital and the outpatient staff on the importance of this, why we were doing this, and how it was going to be done, and that it was safe and that we could do it, was an obstacle. Patient tracking, noncompliance. Patients come one time and have to sit for 3 hours - they are not going to want to come again; and then patients come back to you in a month or so, and you think they have been seen, but then they come back and they have missed all those appointments. So we had to develop a process of catching those patients who were falling through the cracks. You all know what that is like, that happens everywhere.
The office - even before we brought the IV iron into the office, staffing was an issue as I talked about. We had to bring on a few more staff and schedule better for that. Physician and nurse practitioner availability. When we did bring the IV iron to be given in the office, we wanted the physician/nurse practitioner in the office when patients were getting their iron, and actually it was required, so that for us was a comfort measure; it gave us the opportunity to build the relationship with the patient and a lot of times, we killed 2 birds with one stone. They would be there for the office visit and then we give the iron at the same time but that was still an obstacle because you had to work that schedule out because you are still making the hemo rounds and the hospital rounds and peritoneal dialysis rounds. Venous access - we have a wonderful RN and she can almost always hit a vein from here to that wall, but there are always those patients that you know that you have a problem with. Emergency measures were at first not a big thing but you know we did take some emergency measures just in case there was that very rare incident where somebody had a reaction.
12:40

Availability of IV iron therapy
The availability of IV iron therapy. Now that we had the IV iron therapy available to us in the CKD clinic, we had to look at what was out there.
12:51
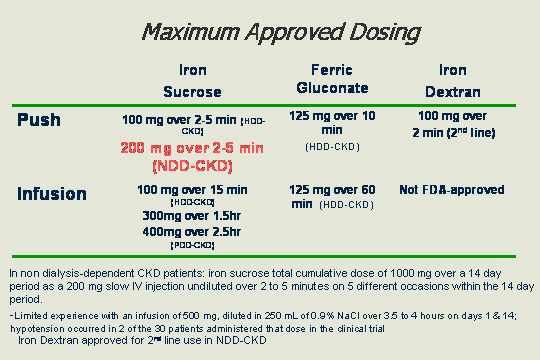
Maximum approved dosing
You are probably familiar with all these, having worked in hemo. Over to the right, you have the iron dextran. It is only approved in CKD clinic for those who fail on oral iron, but we pretty much left that behind due to some reactions to dextran. Ferric gluconate, 125 mg over 10 minutes in the hemodialysis and CKD patients, versus iron sucrose, where we go to 200 mg given using a 2-5 minute push; this does not take long and it is approved in the non-dialysis-dependent CKD patients.
13:26

Protocol development
Let us talk about that a little bit about protocol development. I want to be honest with you. This protocol development is kind of uncharted waters. There was not, especially when we began this, a whole lot of evidence, so we could not call somebody up and say, "Hey, finish your protocol on the IV iron in the predialysis population." And I am not sure that there are many places that you could still call, so we made a few calls before we came here just to see what everybody else is doing.
13:52

Protocol development - a work in progress
So, it is a work in progress. What we looked at was our previous experience - our experience in the hemodialysis unit and the needs. The need of the CKD population who are on the iron is much less than that of the hemodialysis group, and we had to take that into account. We also are experienced with poor anemia treatment response, the compliance issues that we talked about that led to poor response, and then we looked at the patients' needs. What did they need? What would be most convenient for them so that they could be compliant? What do they need based on their level of iron deficiency, monitoring their TSAT and ferritin? How well would they respond to that therapy? Then safety and efficacy.
14:35

Safety
We will go ahead and move over to that. Dr. Reed showed you this slide earlier - showing that, with the 200 mg iron sucrose 2-5 minute push, there were no serious ADEs (adverse drug events). With the 500 mg dose, our experience is really limited; when diluted to 250 mL and given over 3-1/2 to 4 hours, hypotension occurred in only 2 of 30 patients; but our experience with this is limited, and the main finding that we look at is, that there were no ADEs with the 200-mg dose given using a 2-5 minute push.
15:10

Administration of IV iron sucrose - Macdougall study
A study was done by Macdougall in which he administered 2297 injections to 657 patients. As far as what adverse effects he saw, a metallic taste was reported in 412 of those 657 injections and that is not surprising. We all know that, in the hemodialysis patient, we push the iron in and they are like, saying, "What are you doing to me? What is that? I can taste it." It was the same here, but what was interesting was, that upon the second injection, 97.5% reported an uneventful first injection without reactions or side effects. They forgot about it. It was not significant to them.
15:48

Other reactions
Also in that study, 57 patients, 2.5% of the total patients had an adverse event other than the metallic taste; 7 did experience an anaphylactoid reaction, 7 out of 657. However, among those who were rechallenged with 200 mg IV as a 2-hour infusion, there were no adverse events reported. Then the other adverse events were pain during or after injection, nausea, lightheadedness - those type of complaints.
16:22

Time and cost analysis
What was also interesting that they looked was, that it saved the time and cost, and I think that in the world these days, we run a lot on how is the money going to be affected, and how is caregiver time going to be affected. There was a cost saving of over $5000 with the 2-minute push versus a 2-hour infusion. The time required for the 2-minute push was pretty much 5-minutes, where you are drawing up the dose and you are injecting the medicine, and including prep time and everything else. For the 2-hour infusion you need 135 minutes. And so these represent significant differences in time frame required for your day in, day out, activities.
16:59

IV iron alone and/or low-dose EPO in NDD-CKD
One other thing that we looked at when we were looking at protocol development: This is the Silverberg study that Dr. Reed talked about. He looked at IV iron alone or in combination with low-dose EPO, and the target hematocrit of 35% was reached and maintained with iron and low-dose EPO in two-thirds of the patients. What was interesting is that the target hematocrit of 35% was reached and maintained with iron alone in one-third of the patients. So one-third of the patients simply got iron without the EPO and still met target.
17:33
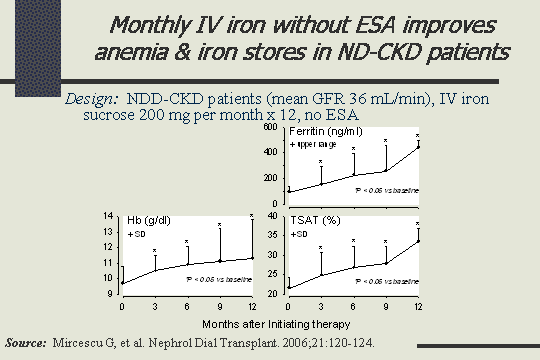
Effect of monthly iron without ESA on NDD-CKD
This has been further supported by a study that was just published this year in the Nephrology Dialysis Transplant journal, and they did a study with monthly IV iron, no EPO, and saw how it affected the anemia and iron stores in the predialysis population, and as you can see there was improvement in anemia and iron stores across the board with 200 mg per month for 12 months, no EPO. The ferritin worked its way up, hemoglobin and the TSAT all began to improve.
18:08
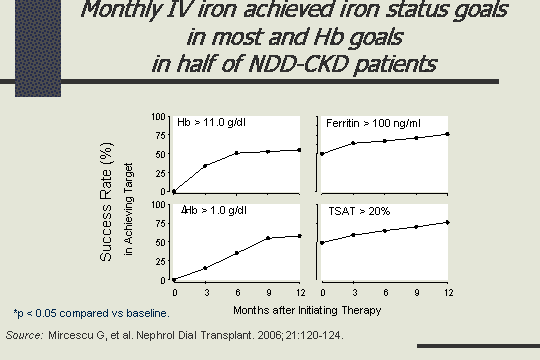
Success rate
Also, not only did they just improve but in terms of hemoglobin goals, in half of these patients, they reached their target. They had a success rate of achieving the target of hemoglobin greater than 11, ferritin greater than 100, TSAT greater than 20%. They did not just improve, the half actually began to meet the targets with iron alone.
18:30
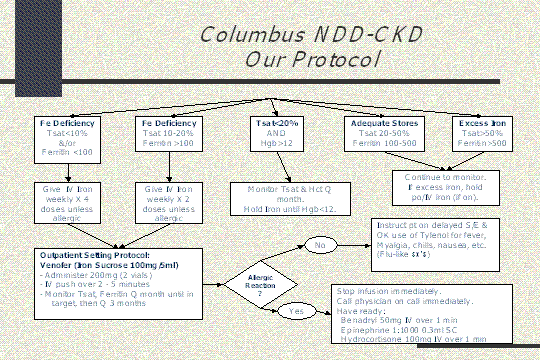
Our protocol
This is our protocol, and I am not going to walk through it step by step simply because the main thing I want you to know about this is, that it is still work in progress. There are still clinical trials, and they are building the protocol, but what we see is that once we establish that the patient is iron deficient, we establish how iron deficient they are, we can determine how much IV iron we are going to give them over what period of time. We get that patient into target. The patients are feeling better, they are in target, they are eating better. They are really maintaining their iron stores very well and what we do in the end is just follow up with the maintenance evaluation of the lab work to see if they needed more iron. They trickle down, we give them a little bit more. At this time, we do not have a specific, okay, this time you are going to miss. We do it based on the patient's needs and what we see with each individual patient because as we know they are all different.
19:28

Conclusions
In conclusion, there are going to be obstacles but they can be overcome. They can be worked through. We have done it in hemodialysis and peritoneal dialysis, and we are still doing it now in the predialysis population. 200 mg of iron sucrose with a 2-minute push in the non-dialysis-dependent CKD patients is FDA approved, and evidence shows you that it's safe for the patient. IV iron is effective in maintaining the iron stores and achieving the hematocrit in this patient population, and there is a protocol development based on the patient's needs as well as the newer evidence which is coming out related to specific efficacy and safety.
20:09

Take-home message
As I said, the take-home message is for you, especially if you know that you are seeing patients in your hemodialysis units, they are not going to CKD clinics, they are not getting their anemia managed, talk to your nephrologists and just ask them if this is in their plan for the future, talk to them about what you have heard here. Realize that if they do begin doing this, your job can be a lot easier but what is most important for us and what was most rewarding and still is for us is seeing the benefit for the patient. Seeing how much better they feel and how much easier the transition is from going from predialysis to dialysis.
In the long run, these are not my babies. I wish they were. I wish I could claim them. These are grandbabies. So, by doing all this, having the lower acuity level, lower hospitalization, we have more time and energy to spend with our families as well.
We are going to get in some questions here. I see that they are taking them up. I am truly honored to be here today to talk to each of you. Like I said, I have worked before, I know what it is like to be that nurse, and I am very honored to be here to talk to you today. Thank you.
00:01
| |||||||||||||