
Cardiovascular Factors in Renal Disease
Dr. Robert N. Foley
May 13, 1997
 |
Robert N. Foley, M.D.
Dr. Foley is Associate Professor of Medicine in the Division of Nephrology at Memorial University, St. John's, Newfoundland, Canada. |

| Synchronized Real Media from Dr. Foley's Presentation | ||

|
 28.8 modem click here to listen! |
You can scroll through the talk while listening to the audio.
There are about 30 slides to this talk.
Download this whole page before
starting up the audio player! The page will automatically
scroll to the slide
being discussed.
You won't be able to listen to these files if you have not downloaded and configured the Real Player (it is built into Internet Explorer version 4.0). To download and configure the REAL player click here. |

Introduction of Dr. Foley by Dr. Carola Grönhagen-Riska:
So we start with the separate session on cardiovascular complications in uremia. As you probably all know, cardiovascular deaths account for 2/3 of all deaths that occur in uremia, both in dialysis and transplantation patients, and these figures have pretty much remained unchanged through the years; about 2/3 still die of various cardiovascular complications; so clearly there is something rotten going on in uremia with the heart and the vasculature. Surprisingly little has been written about this subject, but there is a group in Canada at Memorial University in St. John's, Newfoundland that has done a lot of work within this field and we are very happy to have Dr. Robert Foley here to talk about cardiovascular risk factors in renal disease.
Dr. Robert Foley
Thank you very much. I would like to thank the organizers for this very kind invitation.
Some general comments about Lund and the history of dialysis
I, too, am awed by the history that surrounds Lund. I should probably go back to when I decided to go into nephrology. The first textbook that I very carefully opened was a book which many of you probably know, called Replacement of Renal Function, by the late John Maher. The first chapter that I attempted to read was "Dialysis Biophysics". I soon scrapped that idea and moved on to the history of medicine. I am well aware of the great history that surrounds Sweden, and Lund in particular. I noticed, by the way, that this chapter, "The History of Dialysis", doesn't appear in the latest version. I believe that the editors have changed and now include Kjellstrand, Koch and Winchester. I am just putting a little dig in at Karl (laughter).
Cardiovascular disease is an important cause of death in ESRD
Where I work, we don't have quite the same history. Memorial is a young university. It's been there for approximately 20 years, and our dialysis program has been on the go for a little less than that. In spite of this, I think that dialysis patients are pretty well the same the world over. One of the most striking figures is the presence of cardiovascular disease and the incidence of death due to that. This seems to be the same the world over. Approximately 50 percent of all the deaths in every single registry that I've ever seen are attributed to cardiac disease, which is a staggering figure when you think that countries vary quite a lot internationally in terms of things like myocardial infarction [rates], etc.

(Foley RN et al. Kidney Int 1995; 47:186-192.)The Newfoundland-Quebec Cardiovascular Disease in ESRD Study
Just to tell you a little bit about the study that we've been involved in for many years. This study began in 1982, when I was in second med. It is a pretty long study. The study collected data between 1982 and 1992. It was a prospective study of dialysis patients, all of whom had survived the first six months of dialysis therapy. There was a reason why we elected to pick patients who survived the first six months -- simply we wanted to identify reversible risk factors or something that you could do something about. The data that we collected were a clinical examination and history. We collected mostly data that every dialysis unit in the world collected at that time. We looked at blood pressures, and we looked at hemoglobins and serum albumins, etc.
Now, in addition, at baseline all the patients had an echocardiogram. This was repeated annually for the rest of their life on dialysis. We have very compliant patients, which reflects that the weather is so bad- -our patients have nothing better to do than to go for echocardiograms post-dialysis. I think there is something to be said for bad weather. As you can see, our mean follow up is quite long. This is the principle strength of this study, that it collects data over a long period of time. The three centers involved were two in St. John's--Newfoundland and one in Montreal, in Quebec.
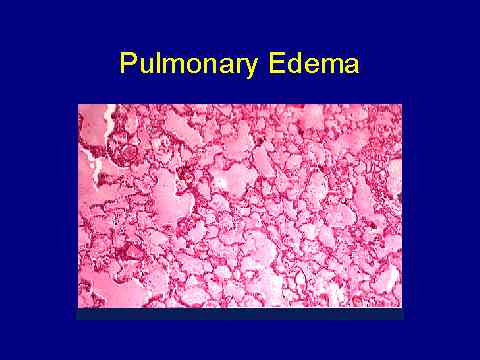
(Harnett JD et al. Kidney Int 1995; 47:884-890.)Cardiac failure is a pre-lethal condition in ESRD
If you want to have a bottom line before you go off to sleep, the bottom line is that cardiac failure is a pre-lethal condition in dialysis patients. About one-third of our patients either had cardiac failure before they started dialysis or went on to get it. When you look at the data after the fact, you find that two-thirds of all of the deaths on dialysis were preceded by an episode of pulmonary edema that required admission. There is always this chestnut about is it actually the heart, or is it actually just fluid overload, or is it both? It's actually impossible to tell clinically often. It's totally impossible in an epidemiological study, but these data are still quite impressive. Far and away in our study, this was the worst thing that you could get. Cardiac failure is a premortem feature of dialysis patients which is, unfortunately, too common.
(EDD = End diastolic diameter, r/Th = cardiothoracic ratio)
(London GM et al. Kidney Int 1987; 32:900-907.LV dimensions and cardiothoracic ratio in ESRD
Dialysis physicians have known for years that our patients have big hearts. So if you go on and do chest x-rays, on average the cardiothoracic ratio (r/Th) is larger than age-matched controls. This is a classic study from a group in Paris from 1987. This group looked at hemodialysis patients. They wanted to be able to separate the non-hypertension and non-ischemic heart related effects out of the picture. They simply excluded the patients with hypertension and a history of myocardial infarction or angina. They looked at the echocardiograms of their patients and compared them to age-matched controls. What they found was that on average the hemodialysis patients, here, had left ventricular dilatation which was more than the general population had. When they looked at associations, they found that the things that were associated with degree of dilatation--anemia, AV fistula, and chronic inter- dialytic excess fluids--these were the factors that were associated. So, again, I suppose that none of this is too surprising.
They then looked at the thickness of these ventricles relative to the degree of dilatation. They found that the dialysis patients tended to have thinner ventricles. So for any degree of dilatation, dialysis patients had a thinner free wall. The only association they could find for this was hyperparathyroidism. So this is a very simple but very classic study.
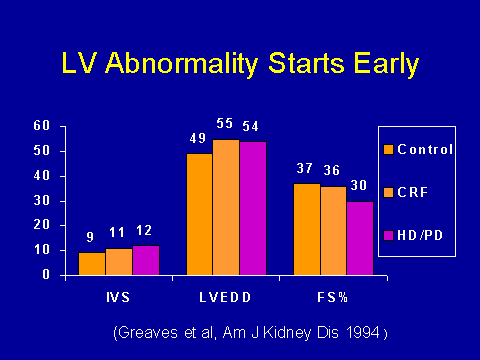
(Greaves et al. Am J Kidney Dis 1994; 24:768-776.LV changes being in the pre-dialysis time period
Countless people have replicated the fact that left ventricular abnormalities are very common if you go looking for them in dialysis patients. That suggests that they start long before the patients get onto dialysis. A number of groups have recently shown this. This is a study from New Zealand. It just shows that the left ventricular hypertrophy, left ventricular dilatation and loss of systolic function start relatively early on. It starts in the pre-dialysis phase.
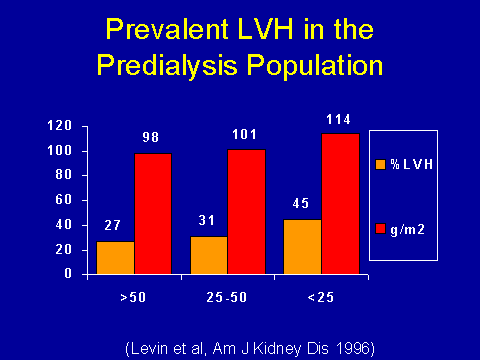
(Levin A et al. Am J Kidney Dis 1996; 27:347-354.This is probably a better study from another group in Canada who looked at pre- dialysis patients in their study, which is identical to ours in other ways. This is a prevalent study, but they have since demonstrated this in a prospective manner. So what you've got on the x axis here is creatinine clearance. I've just shown the left ventricular mass in grams per meters squared and the prevalence of left ventricular hypertrophy. I think you can appreciate that as your creatinine clearance falls, the prevalence of left ventricular hypertrophy goes up. And when they look at this prospectively, they see that large differences can occur within the space of a year and within the space of relatively small decrements in renal function. So this is clearly the time at which things start to go wrong, far ahead of when dialysis treatment starts.
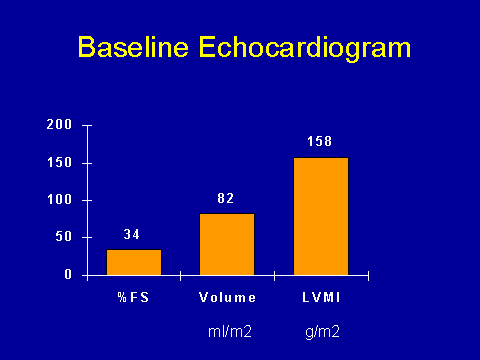
(Foley RN et al. Kidney Int 1995; 47:186-192)In our study, we found that the mean left ventricular mass index was 158 grams per meter squared. The cavity volume was 82 mls per meter squared; fractional shortening, 34 percent. These figures probably don't mean a whole lot to you. In the Frammingham Study, the upper limit of normal for a male is about 130 grams per meter squared; for a female, the upper limit of normal is about 100. Cavity volume is said to be less than 90, and fractional shortening depends upon several factors so there aren't good norms for that.

(Foley RN et al. J Am Soc Nephrol 1995; 5:2024-2031.)Good and bad LV hypertrophy and dilatation
In terms of prognosis, you have to go back to a little balloon physiology to be able to pick out what is really important. As I said, the most characteristic abnormality in uremia is progressive dilatation. If you think of a balloon... I have a cartoon here in diastole. If you go to the law of LaPlace, you find that wall tension goes up as the radius goes up, and it decreases as the wall thickness goes down. So if you're in a state of progressive left ventricular dilatation, you're probably, in terms of the law of LaPlace, better off to have a thicker ventricle.

(Foley RN et al. J Am Soc Nephrol 1995; 5:2024-2031.)In other words, there is good hypertrophy in this situation. Conversely if you've got a problem where it is mostly a thickening phenomenon as opposed to dilatation, maybe you have uncontrolled hypertension or aortic stenosis, you could imagine that a little bit of dilatation would be good for you in terms of wall tension. Just to confuse you even more, you could imagine that if your primary problem is thickening, say you've got this hypertensive cardiomyopathy--the hypertrophy is bad but a bit of dilatation could be good. If you flick over to the people who have dilatation, you could imagine "bad" dilatation and good hypertrophy.
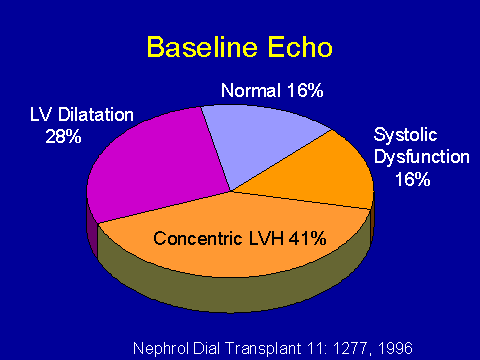
(Parfrey PS et al. Nephrol Dial Transplant 1996; 11:1277-1285.)Echocardiographic findings in the Newfoundland-Quebec study
So once we caught onto this fact, things became very clear and we were able to come up with a slightly modified classification system that was prognostically guided. Basically only 16 percent of our patients could be considered to have a normal echocardiogram. Sixteen percent had a fractional shortening under 25 percent. Concentric hypertrophy was present in 41 percent, and LV dilatation was present in 28 percent. So there is quite a spectrum of abnormality but very little normality.
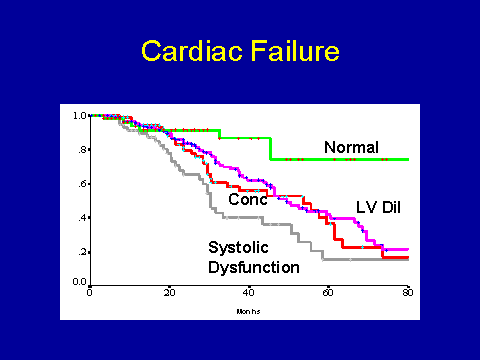
(Parfrey PS et al. Nephrol Dial Transplant 1996; 11:1277-1285.)Effect of LV geometry and function on prognosis
In terms of prognosis, what do these things mean? So what I've got here is the time to first onset of cardiac failure according to the baseline echocardiogram. I would just emphasize that we've excluded patients who had cardiac failure at baseline. You can appreciate that you're a lot better off if your left ventricle is relatively normal when you start. The worst prognosis, as you would expect, is systolic dysfunction. You find that concentric hypertrophy and LV dilatation have an intermediate prognosis in terms of cardiac failure. If you do a similar-type of analysis for new onset ischemic heart disease defined clinically, you get an identical, superimposable picture.
(Parfrey PS et al. Nephrol Dial Transplant 1996; 11:1277-1285.)
If you look at mortality, again it is a very similar picture. You get this gradient of normal, concentric hypertrophy and LV dilatation and systolic dysfunction. Now what you may not appreciate, however, is that the curves really don't start to diverge until about two years after. In fact, having LV dilatation and concentric hypertrophy don't influence your prognosis within the first two years at all. I suppose this isn't unexpected. It also suggests that there is probably, even after dialysis starts a time during which you could perhaps achieve something meaningful for patients.
What about risk factors? I've said that these echocardiographic abnormalities are predictive of future events, and I've said that cardiac failure is very bad for you. You might say, "So what? We can't do anything about it." So when you go looking at risk factors in dialysis patients, it becomes very confusing. It's almost like there is a schizophrenic difference between pre- dialysis and being on dialysis. So one of the things that we are obsessive about in pre-dialysis patients, and rightfully so, is treating hypertension. When we get to the dialysis patients, we don't know what to do, so we go for the worst form of data--we look at epidemiological studies.
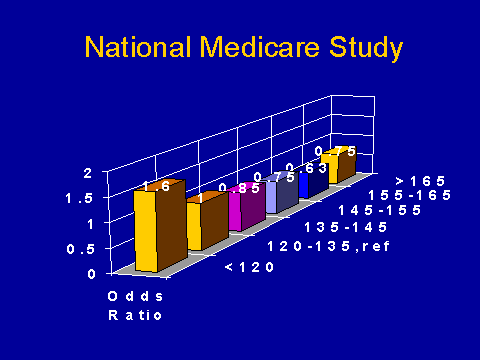
(Lowrie et al. Am J Kidney Dis 1995; 220-228.)Paradoxical effect of blood pressure on mortality in ESRD
This is a study from the United States from Dr. Lowrie's group. They are looking in this particular study at the relationship between blood pressure and subsequent mortality. So it's like a snapshot of blood pressure within the unit. And what I have got here is the odds of dying according to systolic blood pressure. This is adjusted for other factors like anemia, diabetes, age, etc. I haven't mislabelled the slides--this is exactly what the data say. It says that as your blood pressure goes up, your chance of dying goes down; and conversely, as your blood pressure drops, your chance of dying goes up.
Several studies have actually shown similar-type of results. The USRDS and the big Okinawa Registry and the Australian Registry show the same thing. If you take this to the logical conclusion, it's disturbing. Firstly, most hypertension in dialysis patients is volume related, so you have to say to your patients, "Drink more water and take a bit of extra salt." We know that this is illogical.
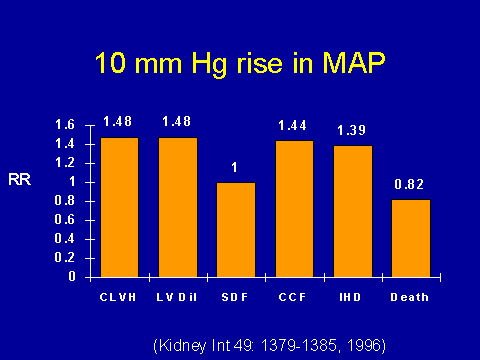
(Foley RN et al. Kidney Int 1996; 49:1379-1385.)Hypertension has adverse effects on LV geometry and function
We had the opportunity to look at this in a more prospective fashion. This is a very busy slide, so I apologize. Our mean arterial blood pressure averaged about 102 mm of mercury for the typical patient measured throughout time. So what I have illustrated here is your risk of dying according to each 10 mm rise in mercury. And again, this is adjusted for all the other bad factors that we think influence prognosis. Again, we get the exact same type of relationship. There is an inverse relationship between high blood pressure and death. However, if you then go and look at all the things that I've said are bad for you, you get the exact opposite. So you see that a rise in blood pressure is associated with the progression of LVH (CLVH), between baseline and the first year, it's associated with progressive LV dilatation (LV Dil) and it's very strongly associated with both congestive heart failure (CCF) and ischemic heart disease (IHD).

(Foley RN et al. Kidney Int 1996; 49:1379-1385.)If you actually look at patients who get cardiac failure, among patients who have had it, the biggest prognostic indicator that they have is low blood pressure. I think what we are seeing is the fact that we have such a heterogeneous population in our dialysis units. I think that hypertension is a major factor that we can do something about it.
Controlling blood pressure in dialysis patients
What can we do about it? We can control it better. Within our dataset in terms of looking at echo and cardiac failure, there didn't seem to be a lower limit to what was the best blood pressure to aim for. Now doing randomized, controlled trials in dialysis patients is a nightmare. I'm only aware of one good study that randomized patients to two different types of antihypertensives.
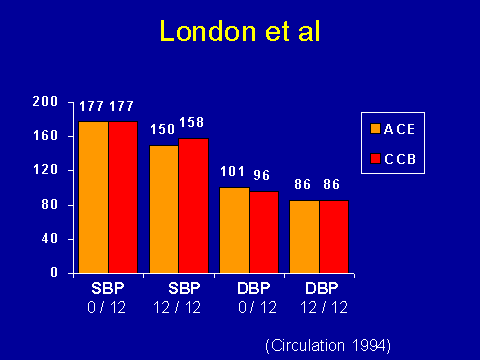
(London GM et al. Circulation 1994; 90:2786-2796.)Again this is from the Paris group. They selected out patients who had uncontrolled hypertension who didn't have ischemic heart disease. These are hemodialysis patients. They simply randomized them to an ACE inhibitor and a calcium channel blocker. They followed them over time. In terms of systolic and diastolic blood pressures, they achieved almost identical blood pressures.
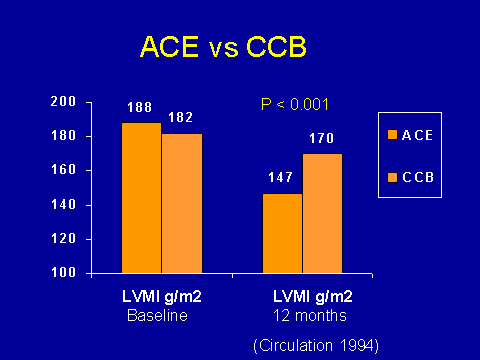
(London GM et al. Circulation 1994; 90:2786-2796.)However, when they looked at left ventricular mass index 12 months down the road, they found that the ACE inhibitor group did significantly better in terms of mass. Now this, again, is a proximate outcome; it's not mortality data. It is a pretty suggestive study all the same, which probably needs to be replicated.
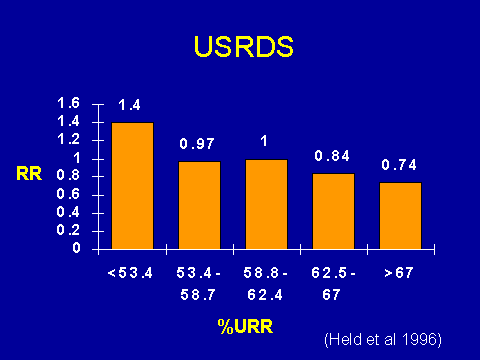
(Held PJ et al. Kidney Int 1996; 50:550-556.Possible effect of dialysis adequacy on LV geometry and function
The other big factor that you see cropping up all the time in the literature is intensive dialysis. You've actually seen this slide this morning. It shows that your adjusted mortality goes up as your urea reduction falls. Again, lots of investigators have shown this, so it's pretty well accepted.

If you go to the animal literature, you find that uremia has fairly pronounced effects on cardiomyopathy, it's a direct myosuppressant--it increases heart size, independently of blood pressure; it causes deposition of ground substance; it kills off myocytes; it causes lower capillary density; and it lowers ATP production. So it seems to be a pretty bad package all around.
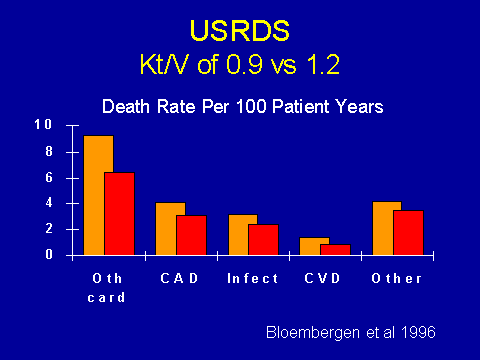
(Bloembergen W et al. Kidney Int 1996; 50:557-565.)Surprisingly little has been written about the influence of dialysis intensity and cardiac outcomes. This, again, is data from the USRDS. They are comparing people with relatively poor Kt/V to those with an adequate Kt/V. You find that cardiac deaths are more common in patients with a low Kt/V. This is the best clinical evidence that we have that uremia is bad for the heart, per se.
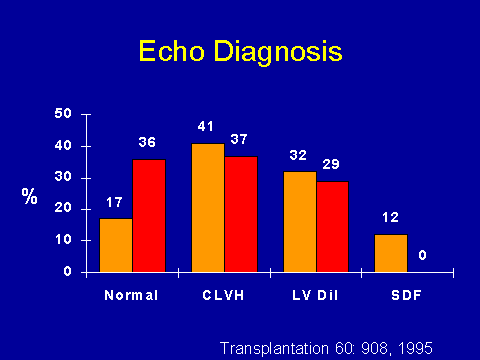
(Parfrey PS et al. Transplantation 1995; 60:908-914.)Effect of transplantation on LV geometry and function
A convenient natural experiment to look at the effect of uremia on cardiomyopathy is to look at people pre- and post- transplant. If you look at the natural history of your typical dialysis patient in terms of echocardiograms, if they stay on dialysis, their echoes stay bad, basically. However, if you look at echoes pre- and post-transplant, you see dramatic differences. We had 100 patients who had an echo within a year of transplantation and more than a year after it. There were pretty profound differences in the echocardiograms pre- and post-transplant. The percentage who ended up having a normal echocardiogram, while nowhere near acceptable, it still was approximately double. The percentage with concentric hypertrophy, about the same: Significantly less LV dilatation but dramatically less systolic dysfunction. So these were patients who might have been not allowed to have transplantation in some institutions. They all had normal coronary arteries as well. But it is a dramatic result.
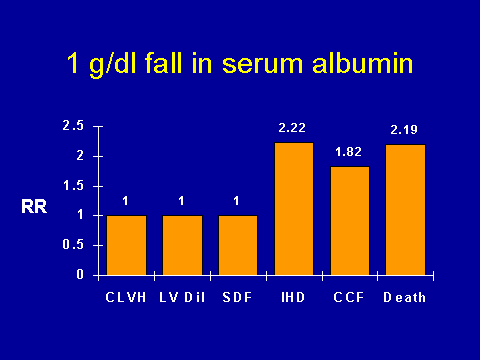
(Foley RN et al. J Am Soc Nephrol 1996; 7:728-736.)Relation between serum albumin and cardiac events
Another interesting finding in this study was the association between low serum albumin and cardiac events. Again, if you're a simple-minded person, this shouldn't be unexpected because of all the variables that have been associated with mortality in dialysis patients, this is probably the most consistent. This is within hemo and peritoneal dialysis patients. So again, we looked at serum albumins prospectively and asked if there was a correlation with cardiac outcomes? In terms of the progression of the cardiomyopathy, there wasn't really a lot of association between a fall in serum albumin and progressive concentric hypertrophy. There was a tendency toward more dilatation if your serum albumin fell. There was a very strong association with new onset ischemic heart disease (IHD) and cardiac failure (CCF) and death. These data are very suggestive that whatever serum albumin is marking for; i.e., that it's mediating some of its bad effects via cardiomyopathy. The million dollar question is: How? I actually can't tell you, believe it or not.

Hemodialysis vs. peritoneal dialysis
One of the more disturbing findings in our study was the disparity in outcome between hemodialysis and peritoneal dialysis patients. So where I live there are a lot of people who live quite a distance away from the institution. We actually do more peritoneal dialysis than hemodialysis. Comparing hemodialysis and peritoneal dialysis patients in terms of mortality is a nightmare because there tends to be an imbalance in major prognostic variables. There is this question about when should the clock start ticking? So, in our study remember that we only looked at patients who survived for six months. There is this question about could there be a multiphasic mortality pattern? You need very long follow up to be able to really give a meaningful answer. Then there is this major problem of crossover between PD and hemo, and how would you analyze that? Having said that, when we looked at the outcomes, there seemed to be a clear disparity favoring hemodialysis, which came into effect at about two years. Serum albumin was the biggest prognostic indicator of this discrepancy. Again, this is worrying data which needs to be confirmed.

(Yang C-S et al. Am J Kidney Dis 1996; 27:380-386.)Anemia as a cardiovascular risk factor
If you move on to anemia as a risk factor, again there is very little written about anemia an mortality in our patients, which is surprising. This is a study from the American Journal of Kidney Diseases. It's from a Japanese study. So after adjusting for age and diabetes, Kt/V, PCR, they found as hematocrit fell, mortality goes up. The range that they looked at was 16 to 36 percent in terms of hematocrit.
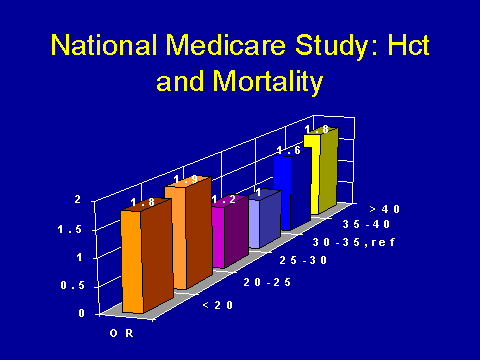
(Lowrie et al. Am J Kidney Dis 1995; 220-228.)This is a study, again it's from Lowrie et. al., and they look at mortality adjusted according to hematocrit. Again, they have what appears to be a U curve. So as your hematocrit drops below 30%, your chances of dying go up pretty dramatically. Worryingly, as your hematocrit rises beyond 35 percent, mortality appears to go up. Again, this is a cautionary note.
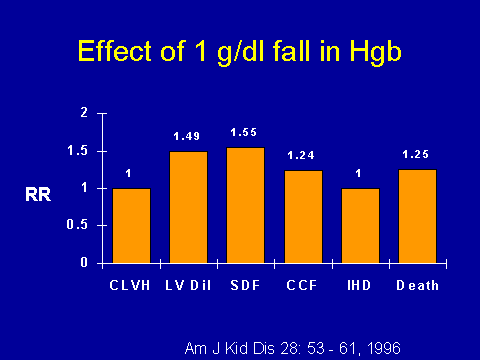
(Foley RN et al. Am J Kidney Dis 1996; 28: 53-61.)Now within our study, our hemoglobin range was between about 75 and 110 g/L, so we can't really extrapolate beyond that. So we measured hemoglobin over time and looked at cardiac outcomes. What you see are adjusted relative risks here and odds ratios. Anemia was very strongly associated with progressive LV dilatation between echos, associated with systolic dysfunction, associated with congestive cardiac failure, and associated with mortality.
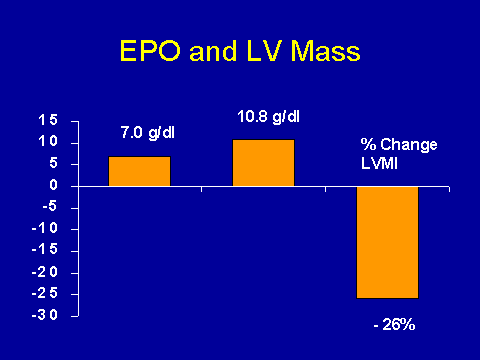
(Muirhead N et al. Am J Kidney Dis 1995; 26(2 Suppl 1): S1-S24.)So this is very consistent with the idea that anemia leads to cardiomyopathy, which leads on to cardiac failure, which leads on to death. This is one of the few things that we can clearly do a lot about. There have been several studies looking at partial normalization of anemia and LV mass. Now, in general, these studies are poor because they don't have a control group so they are just pre- and post-. But the data are very consistent across studies. So if you pooled the studies and you look at percent change of mass index, as you go from an average of 70 (g/L Hgb) before they started treating to 108 (g/L Hgb), approximately 6 to 9 months after treating, does this change left ventricular mass index? All the studies that were referred to there were done in patients already established on dialysis.

If you look at the sequence of events, you go from non-anemic to anemic to cardiomyopathy to cardiac failure and to death, or so it seems to us. And if you believe that prevention is better than cure, you would have to say starting a patient or erythropoietin when they are two years on dialysis doesn't make a whole lot of sense when you could start it a lot earlier.

The optimum level of hemoglobin in ESRD
Another burning question which is quite controversial is: Where should we target our hemoglobins if we accept that treating it is a good thing to do? And if you got 10 nephrologists in a group and sat them down and gave them all a beer and asked them their target, none of them would agree. And if you repeated the exercise in a month, you probably would get 10 different answers from the 10 nephrologists, so you would end up with 100 targets, so nobody really knows.
Most of you will have heard about the Amgen Trial. Now I don't have a slide of it because it is yet to be published. That was a study which specifically targeted hemodialysis patients. They looked at patients who had established cardiac disease within the US. It was a randomized trial. Patients got randomized to current standard therapy, which was a hemoglobin of about 100 g/L, and a more normal hemoglobin of about 130 g/L. They stopped the study early because there was a tendency to higher mortality in the intervention group. They clearly saw an excess of access thrombosis, be it graft or fistula. This is a worrying type of study; however, they did pick a very sick subpopulation. Well over 50 percent were diabetic, and two-thirds had cardiac failure. Obviously they must have picked the group with an unfavorable trade off.

I know many of you are involved in a multi-center Swedish trial. This is a trial that we are involved with in Canada. We're specifically just looking at hemodialysis patients. We have randomized 146 to either a normal hemoglobin target or current standard therapy. Specifically we are looking at patients who don't have ischemic heart disease, who don't have cardiac failure. We should have the first data from this early in 1988. We have been very concerned about safety, obviously, given the Amgen Study. So far we haven't seen an excess of fistula or graft thrombosis.... We are going to look at cost utility formally, and obviously we are checking safety. So the jury is still out on this.

Concluding comments
So I think I've used up my time, and I'll stop at this stage. I suggest to you that uremic cardiomyopathy, though common, is very possibly reversible. We could do a better job, perhaps, of treating uremia. Trying to treat malnutrition is a big issue. We could certainly do better in terms of hypertension. We need to find out what the best agents and best approaches are to do this. We need to find out what is the appropriate target for hematocrits. Once we've done all this, maybe we'll find that the burden of disease has dropped quite a lot.
Thank you for your attention.
References
1. Foley RN, Parfrey PS, Harnett JD, Kent GM, Martin CJ, Murray DC, Barre PE. Clinical and echocardiographic disease in patients starting ESRD therapy. Kidney Int 1995; 47:186-192.
2. Harnett JD, Foley RN, Kent GM, Barre PE, Murray D, Parfrey PS. Congestive heart failure in dialysis patients: prevalence, incidence, prognosis, and risk factors. Kidney Int 1995; 47:884-890
3. London GM, De Vernejoul MC, Fabiani F, Marchais Sj, et al. Secondary hyperparathyroidism and cardiac hypertrophy in hemodialysis patients. Kidney Int 1987; 32:900-907.
4. Greaves SC, Gamble GD, Collins JF, Whalley GA, Sharpe DN. Determinants of left ventricular hypertrophy and systolic dysfunction in chronic renal failure. Am J Kidney Dis 1994; 24:768-776.
5. Levin A, Singer J, Thompson CR, Ross H, Lewis M. Prevalent left ventricular hypertrophy in the predialysis population: identifying opportunities for intervention. Am J Kidney Dis 1996; 27:247-354.
6. Foley RN, Parfrey PS, Harnett JD, Kent GM, Murray DC, Barre PE. The prognostic importance of left ventricular geometry in uremic cardiomyopathy. J Am Soc Nephrol 1995; 5:2024-2031.
7. Parfrey PS, Foley RN, Harnett JD, Kent GM, Murray DC, Barre PE. Outcome and risk factors for left ventricular disorders in chronic uraemia. Nephrol Dial Transplant 1996; 11:1277-1285.
8. Lowrie EG, Huang WH, Lew NL. Death risk predictors among peritoneal dialysis and hemodialysis patients: a preliminary comparison. Am J Kidney Dis 1995; 220-228.
9. Foley RN, Parfrey PS, Harnett JD, Kent GM, Murray DC, Barre PE. Impact of hypertension on cardiomyopathy, morbidity, and mortality in end-stage renal disease. Kidney Int 1996; 49:1379-1385,
10. London GM, Pannier B, Guerin AP, Marchais SJ, Safar ME, Cuche JL. Cardiac hypertrophy, aortic compliance, peripheral resistance, and wave reflection in end-stage renal disease. Comparative effects of ACE inhibition and calcium channel blockade. Circulation 1994; 90:2786-2796.
11. Held PJ, Port FK, Wolfe RA, Stannard DC, Carroll CE, Daugirdas JT, et al. The dose of hemodialysis and patient mortality. Kidney Int 1996; 50:550-556.
12. Bloembergen WE, Stannard DC, Port FK, Wolfe RA, Pugh JA et al. Relationship of dose of hemodialysis and cause-specific mortality. Kidney Int 1996; 50:557-565.
13. Parfrey PS, Harnett JD, Foley RN, Kent GM et al. Impact of renal transplantation of uremic cardiomyopathy. Transplantation 1995; 60:908-914.
14. Foley RN, Parfrey PS, Harnett JD, Kent GM, Murray DC, Barre PE. Hypoalbuminemia, cardiac morbidity, and mortality in ESRD. J Am Soc Nephrol 1996; 7:728-736.
15. Yang C-S, Chen S-W, Chiang C-H, Want M, Peng S-J, Kan Y-T. Effects of increasing dialysis dose on serum albumin and mortality in hemodialysis patients. Am J Kidney Dis 1996; 27:380-386.
16. Foley RN, Parfrey PS, Harnett JD, Kent GM, Murray DC, Barre PE. The impact of anemia on cardiomyopathy, morbidity, and mortality in end-stage renal disease. Am J Kidney Dis 1996; 28: 53-61.
17. Muirhead N, Bargman J, Burgess E, Jindal KK, Levin A, Nolin L, Parfrey PS. Evidence-based recommendations for the clinical use of recombinant human erythropoietin. Am J Kidney Dis 1995; 26(2 Suppl 1): S1-S24.
Back to Nordiska Njurdagar (Nordic Nephrology Days) Meeting Selected Lecture List