|
|
|
 |
The Advancement of Clinical Practice in Chronic Kidney Disease RPA Satellite Symposium March 22, 2002 The Definition and Prevalence of CKD |
|
Dr. Bolton:
The first speaker that we have on this is a gentleman who is well-known for his work in this area, Dr. Bill McClellan who's going to be talking about the definition and prevalence of chronic kidney disease. Bill.
00:00

Dr. William McClellan: Thank you, Kline. Actually I'm going to spend more time talking about where we can find these patients and much less and in fact very little time at all talking about the definition of chronic kidney disease. And the reason for that is that I think one of the most exciting and engaging problems facing nephrology today is the answer to the question "Can we devise a strategy to reverse this epidemic of end stage renal disease that's been occurring in the United States during the last two decades?"
00:00
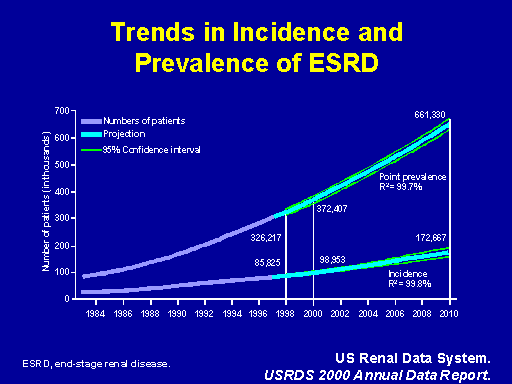
Trends in incidence and prevalence 0f ESRD
This figure taken from the USRDS 2000 annual report is I'm sure familiar to many, if not all, of you. And what it shows is that over the last two decades we've had a steady inexorable increase from year to year in the numbers of new patients who start end stage renal disease or renal replacement therapy. And the other point on this slide is that parallel to the increase in new patients there's been an increase in the prevalent patient population, the numbers of individuals on dialysis at any one particular point in time. If this epidemic increase in incidence continues to occur unabated we're going to see a 50 to 100 percent increase over the next decade in the numbers of new patients starting dialysis. That, in turn, is going to continue to drive the increase in the prevalent population and that aggregate increase in new and existing patients is going to stress the ESRD infrastructure, the nephrology manpower and the financial resources of the Medicare trust beyond anything that we can sustain. And so we have to look at ways to address this epidemic.
Two components of any strategy to reverse this epidemic increase will include a strategy for treating progressive renal insufficiency in ways that delay if not prevent its progression to end stage renal disease, as well as the identification of populations of patients who are at high risk for progression so that we can efficiently and economically target interventions to prevent the progression of this epidemic. Fortunately there's a growing consensus about what we should do with respect to managing the progressive renal insufficiency in patients with chronic kidney disease. And these are being translated into revised guidelines as we speak, by the K/DOQI process.
00:00

Goals of management
Essentially we realize that early recognition of renal injury at a time when we can bring therapy that will effectively stop or at least delay progression is an essential component to this. And this is why we're interested in where these prevalent populations of high risk patients are. When we find them we need to do things to reduce the rate of progression of the chronic kidney injury and that today means tight control of blood pressure, preferential use of an angiotensin converting enzyme inhibitor, particularly in proteinuric patients. And if progression is continuing despite good blood pressure control and ACE inhibition, at least a consideration for dietary protein restriction.
We need to remember the tremendous increased risk for cardiovascular disease that these patients experience. And although we'll hear later this evening that this is primarily a cardiotoxic rather than an atherosclerotic process we do need to identify those patients who are hyperlipidemic and start them on lipid lowering therapy including statins for their hypercholesterolemia.
About the time the creatinine clearance gets in the 60 ml per minute range we know that there's a substantial increase in the prevalence of anemia in the chronic kidney disease population. And that anemia needs to be identified and treated with iron and if necessary erythropoietin. The treatment goals are driven primarily at this juncture by the improvement in quality of life, that reversal of the anemic chronic kidney disease entails. But also a growing appreciation that there may well be a cardioprotective effect or benefit from anemia correction as well.
And then finally if our efforts to control the progression and modify the adverse consequences of chronic kidney disease are of no avail and dialysis is in the offing we need to be sure that we get an early end stage approach to vascular access patients so none of our patients arrive at dialysis with temporary vascular access catheters.
In contrast to this growing consensus about what we should do I think that there are still a lot of questions about where we should be looking for the patients to do it in. And that's what I want to talk about. I want to show you that there are readily accessible populations of high risk chronic kidney disease patients that we should be attending to. And the best way to do that is to contrast the prevalence of chronic kidney disease in the general population to the prevalence in the special populations that I'm going to be discussing in a minute.
00:00

NHANES III
And our information about what's going on in the general population comes from the National Health and Nutrition Examination Surveys. NHANES III is the last completed survey. There's now NHANES IV that is ongoing. And all of the NHANES studies are designed to give us a representative picture of health and disease in the U.S. population. NHANES III was conducted between 1988 and 1994. It was a random sample of the U.S. population. Over 33,000 individuals participated in a history, physical examination and laboratory tests.
00:00
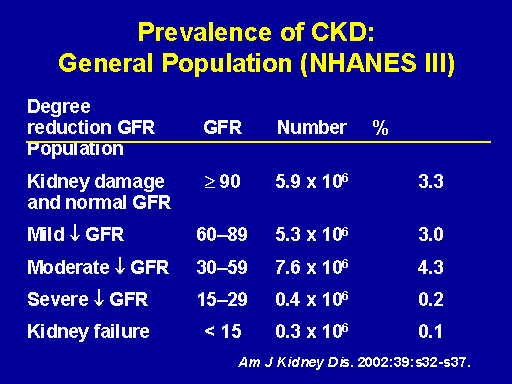
Prevalence of CKD: General population (NHANES III)
And when we look at the prevalence of chronic kidney disease in this population using the stratification that has been suggested by K/DOQI and reviewed by Dr. Bolton what we find is that there's a substantial prevalence of mild to moderate and severe chronic kidney disease in the U.S. population. Now, what I want to do is I want to focus on these moderate to severe patients for a minute because these are the individuals in whom we should be focusing not only our intensive efforts to delay progression but also our attention to anemia treatment and vascular access preparation and so forth. And you can see that between 60 and 30 ml per minute defines moderate decrement in GFR, 30 to 15 ml severe decrement in GFR. And this constitutes about four and a half percent of the U.S. population.
00:00

CKD detection strategies targeted at high-risk populations
This same level of renal function is equivalent to a serum creatinine on the order of about 1.5 milligrams per deciliter. And I want you to keep both that prevalence rate of 4.5 percent and the 1.5 milligrams per deciliter in mind because I'm going to contrast the prevalence in the U.S. population now to several special high risk populations that we as clinicians have ready access to. And those populations include the family members of our dialysis patients, the patients of primary care physicians with whom we interact with on a daily basis and who refer patients to us, and hospitalized patients with diabetes and hypertension and cardiovascular disease. And these are populations that not only are accessible to us and to our colleagues but ones that may well benefit from targeted high risk strategies for the management of chronic kidney disease.
00:00

Family members of ESRD patients: KEEP
The first group, the family members of our dialysis patients we have looked at in Georgia through the National Kidney Foundation Kidney Early Evaluation Program. The KEEP program is a screening program that's being conducted by the NKF through the United States and perhaps some of you in your states as well have participated in it. In Georgia we targeted our KEEP screening at ESRD family members by going to dialysis facilities in ten small cities around Georgia and asking the social worker and the nurses in those dialysis facilities to recruit family members to come in voluntarily for a screen that was conducted either at the dialysis facility site or adjacent to it.
And in those ten regional screens we found that family members who walked through without any preconceived notion about what they were going to receive other than some blood test, 14 percent of them had a serum creatinine greater than 1.5 milligrams per deciliter. This is roughly a three to four fold increase over the prevalence of chronic kidney disease in the U.S. population as defined by NHANES III. Further, one plus or greater proteinuria was present on a random dipstick in 37 percent of this dialysis patient family population. NHANES III found that about one percent of the population had one plus or greater proteinuria. That is, microalbuminuria, macroproteinuria. So this is a substantial increase in the prevalence of proteinuria over what's being observed in the general population. So one potential target population for programmatic activities might be the dialysis patient's family members.
00:00

PAERI study: Case detection in primary care
A second population that is of considerable interest are those patients who are seen by the primary care physician. And these are data from the Prevalence of Anemia in Early Renal Insufficiency Study which is looking at case detection in primary care practices. And what we've done in this multicenter study is sequentially screen patients in over 250 primary care physician practices with a few nephrology and endocrinology practices throw in to leaven the mix. But nonetheless these practices were screened until at least 20 patients with a serum creatinine between 1.5 and six milligrams per deciliter were identified and included in the study.
00:00

PAERI study: Preliminary results
In this early cut at our data ... and we'll soon have a finished report from this study ... of the 123,000 charts that had been systematically screened just over 3,000 or two and a half percent of the patients in the primary care physician's practice had chronic kidney disease as defined by our inclusion criteria. Now, this is actually a lower prevalence than we would expect for moderate and severe kidney disease on the basis of the NHANES III data.
Of course we're using serum creatinine here rather than an MDRD derived creatinine clearance. And so there's a little bit of difference there. But even if we look at the prevalence of serum creatinine 1.4 greater in women and 1.6 and greater in males from the NHANES study the prevalence is over three percent. So the prevalence of chronic kidney disease in these primary care physician practices is actually lower than what we would expect in the general population.
And that doesn't make sense until you realize that what this is an expression of is not a healthier population in these practices but just the lack of systematic searching or screening for kidney disease in high risk patients like their diabetic patients and their hypertensive patients. So one opportunity in primary care is simply to increase the detection through screening for chronic kidney disease.
00:00
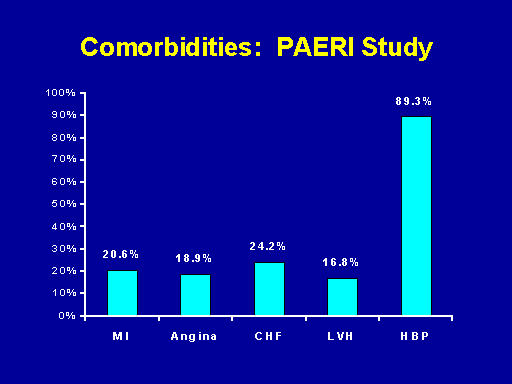
Comorbidities: PAERI study
The important point from the PAERI study, however, is that if a patient in a primary care physician's practice does indeed have chronic kidney disease they have the sorts of complications and comorbid conditions that Dr. Bolton indicated to you was a problem for this population. For example, this is the prevalence of cardiovascular disease in the PAERI cohort participants. And you can see that one in five individuals had a history of myocardial infarction, angina pectoris, heart failure and 17 percent had recorded evidence in their charts of left ventricular hypertrophy. Now, these are not mutually exclusive categories and some people may have had both angina pectoris and heart failure. But the point is there's a substantial burden of cardiovascular disease in these patients with chronic renal insufficiency in primary care. Ninety-seven percent of them, in turn, were hypertensive. So that they clearly are ill.
00:00
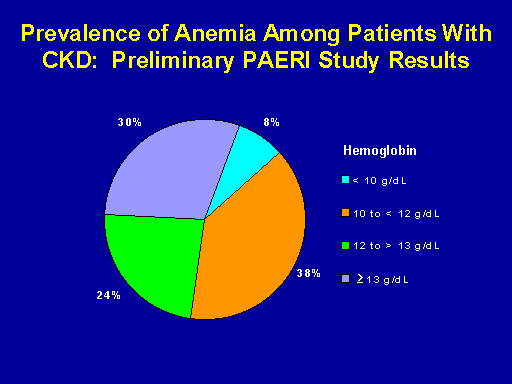
Prevalence of anemia among patients with CKD: Preliminary PAERI study results
Further, when you look at the presence of anemia in this population what you find is that as you might expect given that their creatinine clearances are going to be in that 60 ml and lower range eight percent of them had a hemoglobin of less than 10 grams per deciliter. Another 38 percent had a hemoglobin between 10 and 12 grams per deciliter, substantial prevalence of clinically important anemia in this population.
00:00

Hospitalized patients with high blood pressure and diabetes mellitus
A third population that we have ready access to are those patients who are hospitalized in our community hospitals where we practice and see patients on a day-to-day basis. This is a study that we did in Georgia a number of years ago and in fact Bill Haley, who's in the audience, was one of the integral leaders in this particular study. And what we did in Georgia was we looked at six regional medical centers and academic medical centers and randomly selected 50 charts from people who had been hospitalized either for high blood pressure or diabetes from each of those hospitals and reviewed their charts looking for evidence that a test for either proteinuria, a urinalysis with a dipstick, or a serum creatinine had been conducted in these high risk patients.
And what we found was over half had had a urinalysis and nearly every patient had had a serum creatinine, usually in the context of a multiphasic screening panel. Of those patients who had actually had the test conducted, 29 percent of the diabetics and seven percent of the hypertensive patients had one plus or greater proteinuria. Again, seven to 20 fold difference in the prevalence of proteinuria in these patients compared to the U.S. population. And the prevalence of an elevated serum creatinine of 1.5 or greater was 11 percent of the hypertensive patients and over 14 percent for the diabetic patients. So again a very high prevalence of chronic kidney disease in these patients.
It's reported in the article (but I don't have the slide to show you but I will tell you) that frequently ... in fact, in the overwhelming majority of these patients ... when they were discharged home the presence of the renal abnormalities was not noted in their discharge summary and the more impaired their renal function the less likely they were to go home on an ACE inhibitor and virtually none of them went home on a protein restricted diet, suggesting at least five years ago there was a very low awareness of the need to screen, integrate abnormal screening information about renal function into care plans and translate that into things like ACE inhibition for protection against progressive renal injury.
00:00
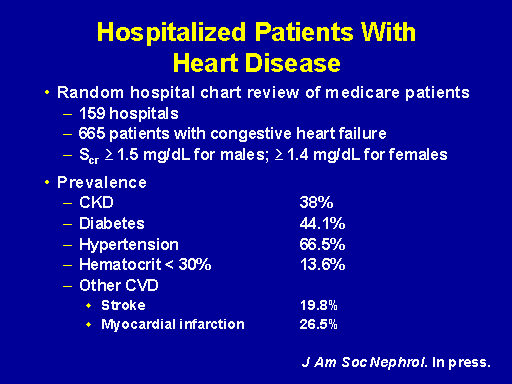
Hospitalized patients with heart disease
This is a study that we did just recently. It was actually in response to some data that you're going to hear, some very important data that you're going to hear later on in this program where we looked at the prevalence of chronic kidney disease in hospitalized patients with heart disease. And in this study in Georgia again and all of the general medical surgical hospitals we randomly selected patients who had congestive heart failure. And in these 665 patients we did a chart review to see if they had a serum creatinine of 1.5 or greater for males and 1.4 milligrams per deciliter or greater for females.
And what we found in this hospitalized heart failure population was that 38 percent of the patients who were admitted with a primary diagnosis and discharged alive with heart failure had chronic kidney disease. An extraordinary prevalence. Further, 14 percent of them were anemic at a level that I think we would all recognize to be clinically significant with a hematocrit less than 30 percent. As you might expect there was a substantial prevalence of diabetes and hypertension and 20 percent of the patients had had a stroke, previous stroke and nearly 27 percent a previous MI.
00:00

Comparisons of CKD prevalence among at-risk groups
So in conclusion we have tools and therapeutic approaches to managing chronic kidney disease and its progression that we need to be bringing to high risk populations. And we can identify those high risk populations. We know where they are. They're the family members of our dialysis patients, the patients we have placed in the hospital that we work at. And to a lesser extent they are the patients who are being seen in the primary care physicians' offices of the colleagues who send us dialysis patients. And we can access those populations with a message that chronic kidney disease is prevalent. It's existent in this population or within these high risk populations and that we need to do something about it if we're going to do anything to delay and eventually reverse this continuing epidemic of renal failure. Thank you.
Discussion:
Audience Member: Bill, in the primary care setting, if you look at high blood pressure and diabetes, how many of those have CKD?
Dr. William McClellan: Yeah. All of the patients in the PAERI study had chronic kidney disease with a serum creatinine between 1.5 and 6.0. So if you were diabetic and in PAERI you had impaired renal function. What we found when we looked at the impact of comorbid conditions in these diabetics, was that they were more likely to be anemic, they were more likely to have poorly controlled blood pressure, and that cardiovascular disease was more prevalent in those patients. So the diabetics had more serious chronic kidney disease than the non-diabetics in the PAERI sample.
Dr. Kline Bolton: But you don't have a feed on if you just look at all diabetics in the primary care practices, what percentage of those would have kidney disease?
Dr. William McClellan: About a third of patients with both type I and type II diabetes will eventually develop clinically significant nephropathy with a proteinuria. And if they survive they'll almost uniformly, as you're well aware, progress to end stage renal disease. But whether the patients who are being seen in primary care practices who are diabetic have a higher prevalence than that one in three -- I don't know the answer to that.
Dr. Kline Bolton: I think you know what I'm driving at. If you're looking at strategies for high risk populations then it would be helpful to know and to be able to give some better guidelines to primary care physicians about screening their diabetic patients. There are a number of good recommendations from the diabetes associations and from the National Kidney Foundation but more data on that would be helpful as well. Because many of these patients, you know as well as I do, are going year by year, coming to the doctor when they have a cold or a sore throat, not getting a lot of routine screening or at best getting something like a blood sugar here or there or a hemoglobin A1c here or there and really aren't getting screened for kidney disease.
Dr. William McClellan: Actually I think that's an extraordinarily important point. And for those of you who are going to be talking to your primary care physicians I'd like to extend it a bit. Not only is the screening being neglected but there is a prevailing belief amongst at least some primary care physicians that if you have a patient on an angiotensin converting enzyme inhibitor there's no need to worry about their kidney function because you've done everything that you possibly can do and that you don't need to be further concerned with screening. At that Georgia Medical Care Foundation where I work we routinely send reports to physicians that detail how they have screened for microalbuminuria or quantitative urine protein as well as glycosylating hemoglobin and lipids on a year to year basis. And we routinely get letters back in response to those report cards saying, "thank you very much, I appreciate this information; but, by the way, I don't screen for kidney disease because all of my diabetic patients are on an ACE inhibitor." So if you take one message away from this particular portion of our talk it is that you need to disabuse your colleagues that you can ignore the renal system just because you have a patient on a particular drug. Even with adequate blood pressure control many patients will still progress. They'll still develop some of the avoidable complications like anemia that are associated with chronic kidney disease and these need to be identified and dealt with as well.
Anton Schoolwerth: Thank you, Bill.
References
1. McClellan WM, Knight DF, Karp H, Brown WW. Early detection and treatment of renal disease in hospitalized diabetic and hypertensive patients: important differences between practice and published guidelines. Am J Kidney Dis. 1997 Mar;29(3):368-75.
| This educational activity is supported by an educational grant from Ortho Biotech Products, L.P. This activity has been planned and produced in accordance with the ACCME Essential Areas and Policies and with CE policies of the State of California Board of Registered Nursing. From a CME Symposium held on March 22, 2002 at the Renal Physicians Association (RPA) Annual Meeting in Washington, DC. This symposium was approved by the RPA. It was not part of the official RPA Annual Meeting as planned by the RPA Program Committee. |
| |||||||||||||||