|
|
|
 |
 |
 |
| |||||||||||||||||||||||||||||||||||||||||||
00:01

Introduction
Dr. Reed is a practicing nephrologist in Columbus and he trained at UMC and UAB in Alabama, and he is actually the Medical Director of five dialysis units and one acute hospital. Dr. Reed likes to be known as a doctor who works. He works very well with the nurses. He is in day-to-day contact with nurses, so he understands the day-to-day routine of dialysis units. He understands the problems we all have as nurses, and you will be able to see that in his presentation.
Dr. Reed
Thanks to ANNA and to American Regent for your sponsorship. It is always a pleasure and an honor to be with the nurses. I think this group multitask better than anybody in any medical industry, and hats off to you for what you do everyday for our patients. Betsy and I will talk with you today about a new direction that we have taken in our iron management in the CKD or predialysis area and for definition purposes where you see the NDD (non-dialysis-dependent), we are basically talking about predialysis patients.
01:22

Objectives
These are objectives, and I will go over the trials, particularly looking at oral iron therapy versus IV, and Betsy will review the obstacles to success and protocol development.
01:34

Outline
First I will have a general review of non-dialysis-dependent CKD patients and anemia, and then we will get into the use of IV iron in this population.
01:49
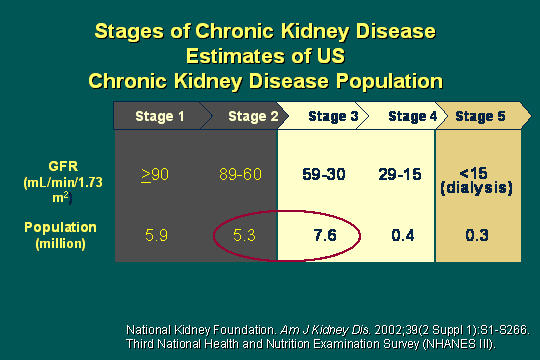
Stages of CKD
These are the stages, and I think most of you are very familiar with this. These are the stages of chronic kidney disease and the estimates of prevalence throughout the United States. If you look at this prevalence, we are talking about 20 million people that are afflicted by some form of chronic kidney disease. To go through them by stage and GFR, GFR being simply a measurement of remaining kidney function, you can generally see that from 0 to 100 that represents the remaining function the patient would have.
For stage 1, that is, someone with very minimal disease with GFR over 90, there are about 6 million people in that group. For stage 2, GFRs are 60-89, just about 5 million people in that group. For stage 3, where GFR is 30 to 59, there are about 7.6 million people. Note the big change to stage 4 - 400,000 people with GFR 15-29 and look at stage 5, which are the patients I assume most of you are seeing in dialysis units, with GFR under 15, only 300,000 to 360,000, I think, is the number today. So the big question is, what is happening to stage 4 and 5 patients?
03:22
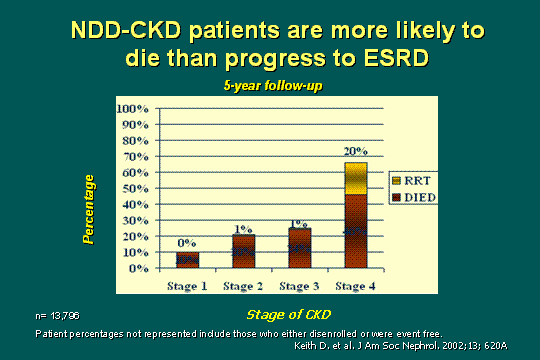
High mortality in NDD-CKD
I think if you look at the patients you see who enter the dialysis unit and who have not been seen in the clinic for predialysis treatment, you know the answer very well. These patients are dying before they ever get to ESRD and in a sense it is only the lucky ones that make it to this point. As you can see by stage and by percentage at stage 4, there are more people dying than reaching dialysis. The group that is not mentioned there, in this Medicare 5-year follow-up is the event-free. If you put them in, it would be even more impressive as to the number that really come to see us in the dialysis unit.
04:06

Slowing progression
This is a slide that I have put in at the last minute because I like in the CKD talks with my referring physicians, to think about what is it that I can do to slow the progression of chronic kidney disease as a whole and no question the top 3 are our big targets, antihypertensive therapy, management of the anemia, and proteinuria. We will look at anemia today as a very important risk factor in slowing the disease process and for all these we do have very good data. We will look at the biggest problem with early referral and that is being able to get the patient and we could talk all day on that, but I will just say that is one of the challenges that we all have in nephrology - getting to that patient in time to do something for him, so he may not need to come from the hospital to the dialysis facility.
05:06
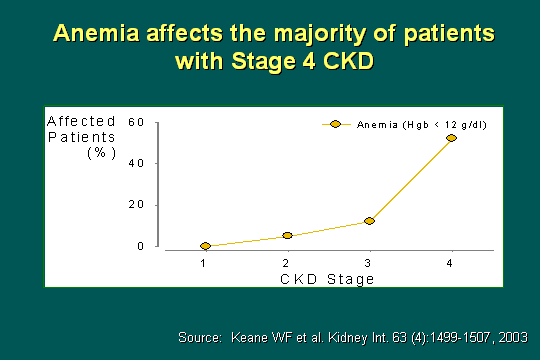
Anemia in stage 4 CKD
How prevalent is anemia in stage 4 CKD? You can see that by percent affected by stage; clearly, with hemoglobin less than 12, more than half the patients in stage 4 are affected by anemia.
05:28
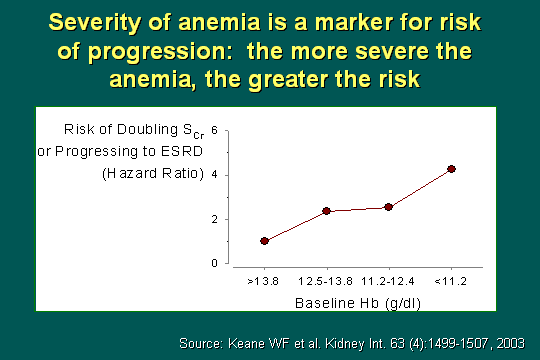
Anemia and progression
How does severity rank as a marker for risk of progression? If you look at the baseline hemoglobin, as it worsens from 13.8 to 11.2 on the right and you plot that against the risk of doubling of the creatinine, which was pointed out in the RENAAL study several years ago, but it is still very important data, there is a very linear relationship; and if you look at the patient with a Hb less than 11.2 and follow that up and over to a hazard ratio of the risk of doubling (the serum creatinine), there is a 4 times greater chance of progressing to ESRD when the hemoglobin is less than 11.2.
06:19

Causes of anemia in NDD-CKD
If anemia is the big problem that is predicted here, what can we do about it and what are the causes? Unquestionably, as the kidney shrinks, EPO deficiency sets in, but the secondary causes of iron deficiency, inflammatory condition, and hyperparathyroidism are also very important. Today we will talk about iron deficiency and what causes it and how prevalent it is, and what we can do about it.
06:52
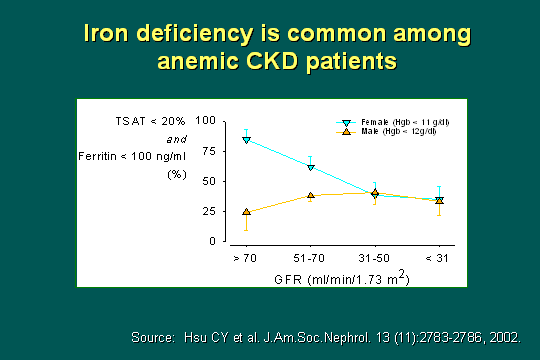
Iron deficiency is common
This slide is a little bit complicated but if you just look at the blue line, it shows the females and the yellow is the males; as kidney function deteriorates, look at the TSAT under 20 and ferritin under 100: You can see by gender and kidney function, that there as many as 20% to 70% of people that are iron deficient by these criteria, and obviously the females having larger blood loss, but by stage 4, or with a GFR in this case of 30 to 50 by this study of NHANES data, you can see that 40% to 50% of all patients are deficient in iron. Now you might say, 40% how big is that? The point being, what is the percent incidence of this in matched controls - in males for instance? It is less than 1%. So there is a 40 times higher incidence of iron deficiency when you add CKD into the formula.
08:11

Causes of iron deficiency
What are the causes of iron deficiency? First on the list in our clinic is bleeding, and most of this is GI bleeding that goes with the territory, so you see a very sick patient with lots of problems. Second is impaired absorption, which may be due to lack of intake from poor intake of iron-containing foods. If they have been to our clinic and we find a high phosphorus, we compound the problem with our binders, which may bind up the oral iron. Finally, the ESAs or erythropoietin-stimulating agents, clearly increase the demand for iron. Where is the iron in the body? It is in the blood, and as the ESA agents stimulate blood making, there is no question of the huge demand for more iron to be mobilized. Keep that in mind as we go into the presentation on IV versus oral iron, and how much reserve iron you have, because when you start EPO there is a tremendous demand for more iron.
09:31

Iron treatment options
We will go into the references (studies) here on when iron is given alone or with the EPO; which is better in this population? We will also look at oral versus IV iron, and what is the evidence for one or the other?
09:52
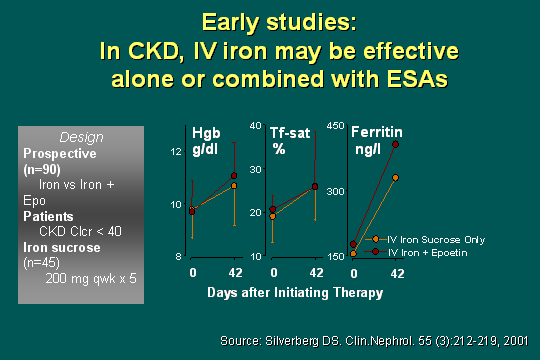
Early studies of IV iron in CKD
The early studies and this study by Silverberg some years ago in 2001 is a little complicated, but if you look at the light line, that is iron sucrose only, and the darker line on top of each slide is IV iron plus EPO. At that time, this was a 6-week study, about 42 days, looking at the hemoglobin between 8 and 12, there was unquestionably a significant rise in all targets - hemoglobin, iron saturation, and ferritin. If you read the paper further, one-third of these patients with iron sucrose only, needed no EPO. I think that is a very important point that we need to point out in the chronic kidney disease clinic, given the difficulties we have in coming up with ESA agents, and Betsy will tell you more about that.
11:01
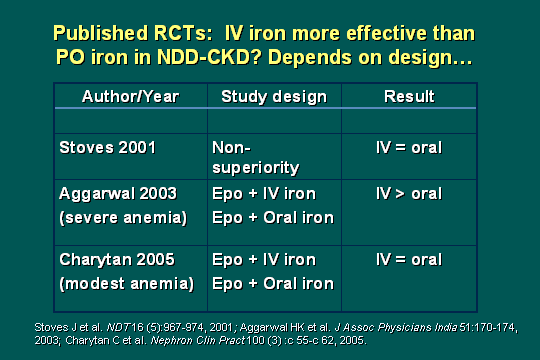
Published RCTs
Prior to a few months ago, these were the 3 randomized trials that have been published on whether IV iron was more effective, less effective, or equal, to oral iron in the non-dialysis-dependent CKD patients. What the studies showed is that the IV iron was equal to oral iron in 2 of the 3 studies, and IV iron was better in 1 study. This has already been proven in your dialysis population, and your own Becky Wingard who I think is with us today, published studies on the hemo and PD patients years ago, that IV was better. So where is the evidence now with this conflicting data today, probably largely due to iron problems? There was a need for another study.
11:57

IV vs. oral iron in CKD: Van Wyck
Dr. Van Wyck published this study a few months ago in Kidney International. Basically he took a new approach and did a randomized trial comparing IV to oral iron, and he looked at oral iron for 6 weeks with ferrous sulfate 325 mg 3 times per day and IV iron either by 200 mg push or by an infusion of 500 mg over 3-1/2 to 4 hours. The patients were rigidly controlled; they had to be in stage 3 to 5, hemoglobins had to be less than 11, TSATs less than 25, and ferritin less than 300. What was different in this study from the others that helped control for variables is, that these patients either had no EPO, or the EPO was not changed during the 6 weeks' time, and the evidence was much more clear and, I think, answers the question.
13:05
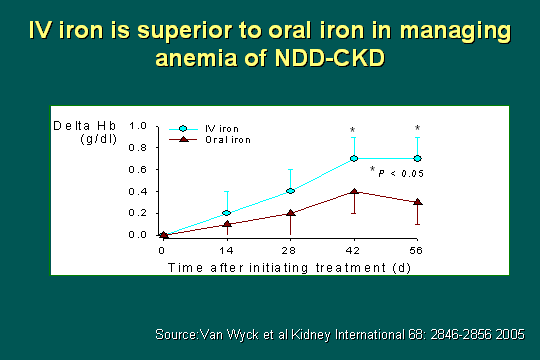
Delta Hb data
We will go through the individual slides, but as far as the IV iron being superior to oral in managing anemia across the board, obviously our biggest indicator would be the delta hemoglobin and in this case, a rise in hemoglobin of 1 point (g/dL) and over the 56 days of treatment; you could clearly see that IV iron was superior to oral iron.
13:35
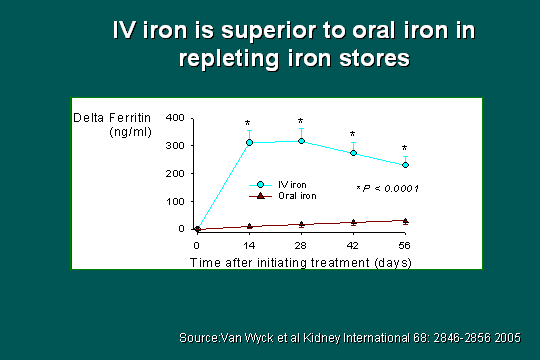
Ferritin data
Looking at the stores, as I told you, it is very important that we have iron stores available, particularly when initiating ESA. To get the ferritin into the range of 200-300, the IV iron was far superior, no question. If you look at the bottom line here, the red line, the time from initiation to the end of the study, oral iron never made the target. I think we have gone through the same process that Becky did with the dialysis-dependent patients, and we have come out with the answers here, and I will show you some more ways to look at this.
14:20
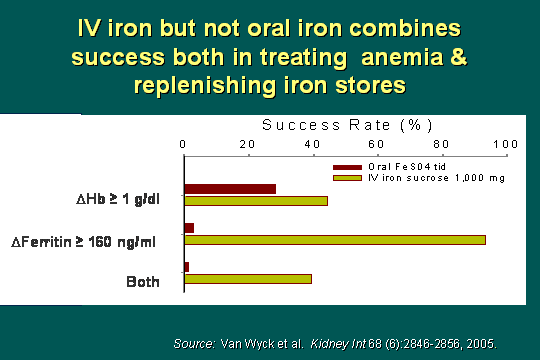
Hb plus ferritin
In summary, if you look at the delta hemoglobin, there is no question that IV is better, and in ferritins over 160, better; but looking at both together, there is a remarkable enhancement of outcomes here with IV iron over oral in terms of success rate.
14:45
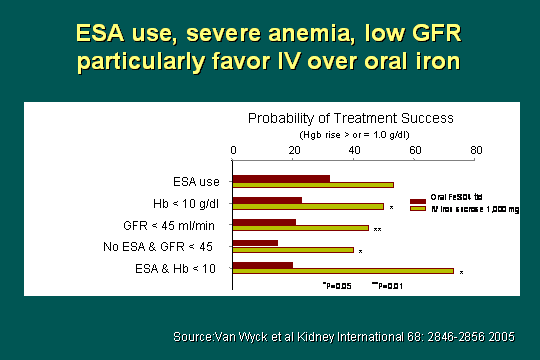
Factors determining treatment success
What factors are important here in determining probability of treatment success? This is pretty straightforward, but again: 1) EPO use, 2) severity of anemia, with hemoglobin over 10, and 3) GFR under 45. If you look at combinations (of outcomes), most combinations showed even more effect: e.g., no EPO with GFR under 45 - a very, very high probability of treatment success. Taking that most severely anemic patient, hemoglobin under 10 with initiation of EPO - that was the group that had the most benefit of all.
15:37

Safety results
In terms of safety, Betsy will talk more about this in protocol development but the 200 mg (IV iron sucrose) push is now FDA approved, and there were no serious adverse events in Dr. Van Wyck study, and I think that is very comforting to us in the CKD clinic, and we found that same experience as we have administered a great deal of this over the last couple of years.
16:11

Clinic outcomes
I would like to end by giving you some of our outcomes, so to speak - real-world outcomes. This is data that was collected by my colleague here over a 3-year period, 2002-2004, in our own clinic, and I want you to get a sense of what the CKD clinic concept as well as anemia management can do for patients that are coming to you. This is where I would like to try to tie the importance of the CKD clinic and the anemia management together for you and the patient. I think you very clearly see what it has brought.
16:51

1st 90-day hospitalization
Here you can look at first 90-day hospitalization, and the percent of patients, on the vertical axis, as a function of whether they were patients in our clinic or not in our clinic, and whether or not they had anemia management; you can see that 33% of this garden variety of people who were started on dialysis had hospital days, compared to 11% if they actually came to our CKD clinic; and if you add treatment of anemia in any way you want to define it, we were down to 8%. So there is a four-fold decrease in the first 90-day hospitalization and for the acuity of problems that we see, I think that is a real remarkable outcome, and we are very proud of that.
17:45
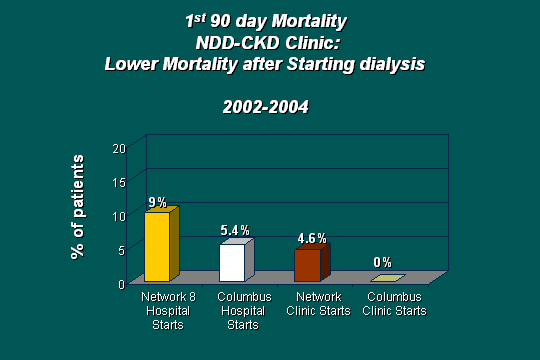
1st 90-day mortality
As far as mortality, which is the bottom line here - can we save lives with this approach? If you look at what our outcomes were by site, whether we had seen the patients and compared them to Network (clinic versus hospital), you see in the first yellow bar that Network Hospital starts had about a 9% overall mortality. In our hospital starts, we did a little better, 5.4%, and we think that is because we have been out talking about this, and we had less of it. We actually decreased hospital starts about 75% during this period of time. If you look at the Network Clinic starts, mortality is about 4.6%, and if you look at our Columbus Clinic starts - the patients that we followed in the CKD Clinic - at the end of this 3-year study we did not have a death. We are very excited about that. It gives us lots of energy to go on and push this program outside the dialysis unit and our own practice.
18:58
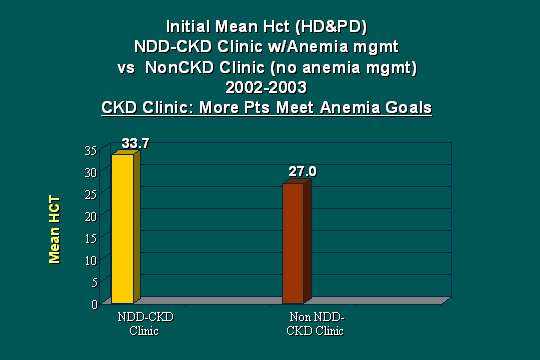
Initial Hct: Effect of CKD clinic
Now you say what is in this for the anemia managers? And how excited they are about this in our PD and our hemo units! If you look at the mean hematocrit in the CKD clinic, the patients that we saw, the mean was 33.7% and for those that we did not see, it was 27%. Why? Does that make a difference, bringing somebody in that well and how well do we know that anemia is such a marker of hospitalization rate and marker of mortality? So our anemia managers were very excited when we began to send in patients that had these kind of numbers.
19:48
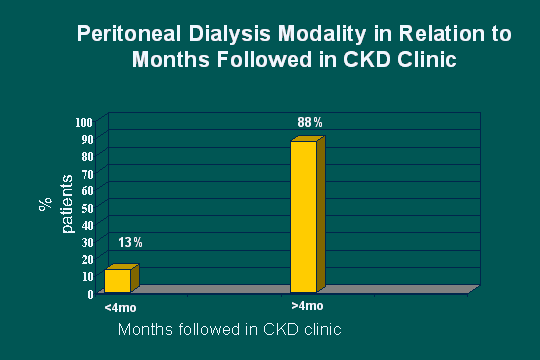
Choice of PD vs. CKD clinic followup
As far as PD, do we have PD nurses here today? Great. This is a slide that again I take a lot of pride in but I have to give the credit to this lady on the right. The choice of PD modality relating to the number of months we have followed them, and you see in the first bar, the low bar, 13%. If we did not see a patient for more than 4 months, we had little chance of impacting their modality, whereas more than 4 months, 88% chose peritoneal dialysis. How many actually went to PD - is it in the 50% range? And these numbers conflict rather significantly with published data of 50% and 35%, but I will tell you what my assessment of this is.First of all I believe that these patients saw us long enough even though 4 months does not seem like very long. If you have things done to them, you make them feel better and if you think about those uremic patients that we see in the hospital, I am not sure they are thinking well enough to know what we are talking about. With correction of anemia, we carry more oxygen into the brain. I propose that they can more clearly make a decision. Then I think after they feel better, they develop a trust with the whole team and more Betsy than me because she spends more time with them and really develops that relationship that it takes to lead a patient to do what you think is best for them and for them to have that opinion. So our PD nurses have been very happy with this.
21:47
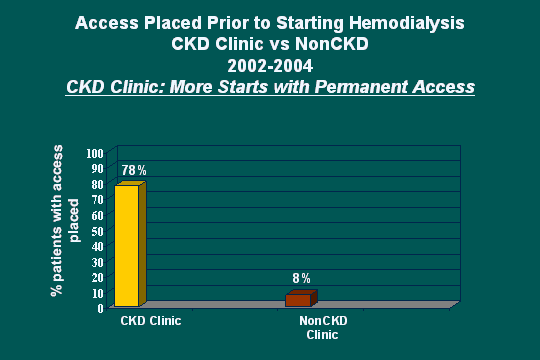
Access placed vs. CKD clinic followup
As far as the hemo nurse, I think this is the really big slide, access placed prior to starting dialysis. About 78% of the patients in this study were able to go to hemo with an access in place, and we are very proud of that and as you can see with people that did not come to clinic, we still got a few accesses in but not near what we did in the clinic outcome. You might say what does this have to do with anemia? This is just a spinoff. This is another outcome that related to the overall program that we have.
22:30

Conclusions
In conclusion, anemia does affect the majority of patients in stage 4 CKD, iron deficiency is very common, and IV iron is superior to oral iron in this predialysis group of patients and from our own clinic slides, you can see the improved outcomes are seen with anemia management and all the things that it let us to be able to do while we followed these patients. I will turn it over to Betsy now, and she will tell you more about how we made this happen and developed a protocol.
References
- National Kidney Foundation. K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classification, and stratification Am J Kidney Dis. 2002 Feb;39(2 Suppl 1):S1-266.
- Keane WF, Brenner BM, de Zeeuw D, Grunfeld JP, McGill J, Mitch WE, Ribeiro AB, Shahinfar S, Simpson RL, Snapinn SM, Toto R; RENAAL Study Investigators. The risk of developing end-stage renal disease in patients with type 2 diabetes and nephropathy: the RENAAL study. Kidney Int. 2003 Apr;63(4):1499-507.
- Hsu CY, McCulloch CE, Curhan GC. Iron status and hemoglobin level in chronic renal insufficiency J Am Soc Nephrol. 2002 Nov;13(11):2783-6.
- Silverberg DS, Blum M, Agbaria Z, Deutsch V, Irony M, Schwartz D, Baruch R, Yachnin T, Steinbruch S, Iaina A. The effect of i.v. iron alone or in combination with low-dose erythropoietin in the rapid correction of anemia of chronic renal failure in the predialysis period. Clin Nephrol. 2001 Mar;55(3):212-9.
- Stoves J, Inglis H, Newstead CG. A randomized study of oral vs intravenous iron supplementation in patients with progressive renal insufficiency treated with erythropoietin. Nephrol Dial Transplant. 2001 May;16(5):967-74.
- Aggarwal HK, Nand N, Singh S, Singh M, Hemant, Kaushik G. Comparison of oral versus intravenous iron therapy in predialysis patients of chronic renal failure receiving recombinant human erythropoietin. J Assoc Physicians India. 2003 Feb;51:170-4.
- Charytan C, Qunibi W, Bailie GR; Venofer Clinical Studies Group. Comparison of intravenous iron sucrose to oral iron in the treatment of anemic patients with chronic kidney disease not on dialysis. Nephron Clin Pract. 2005;100(3):c55-62. Epub 2005 Apr 11.
- Van Wyck DB, Roppolo M, Martinez CO, Mazey RM, McMurray S; for the United States Iron Sucrose (Venofer) Clinical Trials Group. A randomized, controlled trial comparing IV iron sucrose to oral iron in anemic patients with nondialysis-dependent CKD. Kidney Int. 2005 Dec;68(6):2846-56.
00:01
| |||||||||||||